Proximal humerus fractures (PHFs), including humeral head fractures, are common injuries, particularly in elderly populations, often resulting from low-energy trauma such as falls. Management strategies vary depending on fracture complexity, patient age, bone quality, and functional demands. While many minimally displaced fractures are treated nonoperatively, complex and displaced fractures frequently require surgical intervention, most commonly open reduction and internal fixation (ORIF) with locking plates, intramedullary nailing (IMN), or shoulder arthroplasty.
Operative fixation aims to restore anatomy and provide stability to allow early mobilization, which is critical to prevent complications such as stiffness, frozen shoulder, and muscle atrophy. Postoperative rehabilitation is a vital component influencing functional outcomes. However, there is considerable variation in rehabilitation protocols, including immobilization duration, timing of passive and active range of motion (ROM) exercises, weight-bearing restrictions, and use of manual therapies. Different type of surgical fixation is also one of the key components of decision making for rehab plan.
This protocol synthesizes current evidence and expert consensus to guide clinicians through an evidence-informed, phase-wise rehabilitation program following operative management of proximal humerus fractures.
Phase 1: Immediate Postoperative Phase (0-2 weeks)
- Timeline: Postoperative day 1 to 2 weeks
- Goals:
- Protect surgical fixation and promote fracture healing
- Manage pain and inflammation
- Prevent stiffness in adjacent joints (elbow, wrist, hand)
- Maintain patient independence in activities of daily living (ADLs) within precautions
- Immobilization:
- Shoulder immobilized in a sling or brace, worn continuously except during exercises or hygiene
- Immobilization duration varies but often ranges from 1 to 3 weeks
- Precautions:
- No active shoulder movement or lifting
- Avoid shoulder extension, abduction, and external rotation beyond pain tolerance
- No weight bearing through the operative arm
- Interventions:
- Patient education: Sling use, activity modification, pain management
- Exercises:
- Pendulum exercises (gentle, passive shoulder motion)
- Passive ROM (PROM) within pain-free range, initiated as early as 1-2 days post-op, especially in minimally displaced fractures or stable fixation
- Isometric contractions of scapular stabilizers and deltoid muscles without shoulder movement
- Active ROM (AROM) of elbow, wrist, and hand
- Breathing exercises and postural training
- Criteria to progress to Phase 2:
- Pain controlled with minimal analgesics
- No signs of fixation failure or complications
- Ability to perform PROM and distal joint AROM without increased pain or swelling
Phase 2: Early Mobilization Phase (2-6 weeks)
- Timeline: Weeks 2 to 6 postoperatively
- Goals:
- Gradually restore passive and active-assisted shoulder ROM
- Minimize stiffness and adhesions
- Continue protection of fracture site
- Immobilization:
- Sling use may be reduced gradually, typically worn only for comfort or during ambulation
- Begin to discontinue immobilization by end of this phase, depending on fracture stability and surgeon’s guidance
- Precautions:
- Avoid heavy lifting (>1-2 lbs)
- Avoid shoulder elevation beyond 90° initially
- No resisted shoulder movements
- Interventions:
- Exercises:
- Passive shoulder ROM progressing toward full range as tolerated (flexion, abduction, external and internal rotation)
- Active-assisted ROM (AAROM) exercises (e.g., wand exercises, pulleys)
- Scapular stabilization exercises (e.g., scapular retractions, scapular clock)
- Isometric strengthening of rotator cuff and deltoid without resistance
- Continue active elbow, wrist, and hand exercises
- Manual therapy: Gentle soft tissue mobilization and massage to reduce adhesions and improve tissue extensibility may be added if available
- Exercises:
- Criteria to progress to Phase 3:
- Achieving near-full PROM without pain
- No signs of fracture displacement or hardware complications
- Ability to perform AAROM exercises effectively
Phase 3: Active Motion and Strengthening Phase (6-12 weeks)
- Timeline: Weeks 6 to 12 postoperatively
- Goals:
- Restore active shoulder ROM
- Initiate strengthening of shoulder and periscapular muscles
- Improve neuromuscular control and proprioception
- Immobilization:
- Discontinue sling use
- Precautions:
- Avoid lifting heavy objects (>5 lbs) until cleared
- Avoid sudden jerky movements or overhead activities causing pain
- Interventions:
- Exercises:
- Active ROM (AROM) exercises in all planes, gradually progressing to full range
- Resisted isometric exercises progressing to isotonic strengthening with light resistance (e.g., Theraband, light weights starting at 0.1 kg progressing to 0.5 kg)
- Closed kinetic chain exercises (e.g., wall push-ups, weight shifts)
- Scapular strengthening (e.g., rows, scapular punches)
- Proprioceptive neuromuscular facilitation (PNF) techniques and neuromuscular re-education
- Functional task training (e.g., reaching, lifting light objects)
- Manual therapy: Continued soft tissue mobilization and joint mobilizations as indicated
- Exercises:
- Criteria to progress to Phase 4:
- Active forward elevation to at least 120°
- Strength at least 50% of contralateral side without pain
- Radiographic evidence of fracture healing
Phase 4: Advanced Strengthening and Return to Activity Phase (3-6 months)
- Timeline: 12 weeks to 6 months postoperatively
- Goals:
- Restore full strength and endurance of shoulder girdle muscles
- Return to work and recreational activities safely
- Achieve functional independence without pain or instability
- Immobilization: None
- Precautions:
- Avoid contact sports or heavy lifting >10-20 lbs until fully cleared
- Avoid activities causing pain or discomfort
- Interventions:
- Exercises:
- Progressive resistance training with increased load and complexity
- Plyometric and dynamic stabilization exercises
- Sport- or job-specific functional training
- Endurance exercises for shoulder and upper extremity
- Stretching exercises to maintain flexibility
- Exercises:
- Criteria for discharge:
- Full, pain-free ROM comparable to contralateral side
- Strength at least 80-90% of contralateral side
- Patient able to perform functional tasks relevant to lifestyle or occupation
- Radiographic union confirmed
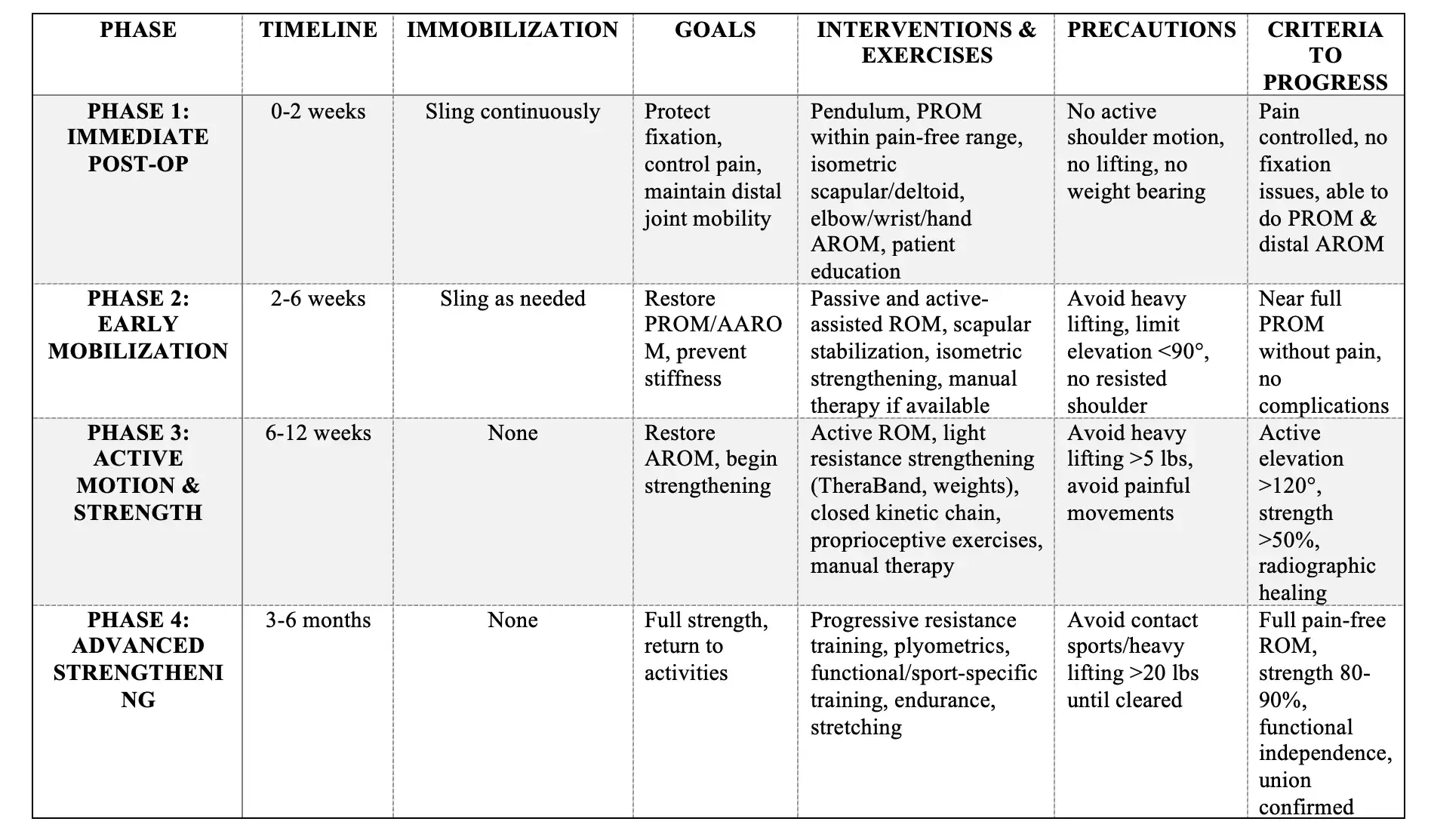
Summary Table of Rehabilitation Phases
Key Points from Literature
- Early active motion protocols following ORIF with locking plates are not inferior to restrictive protocols and may improve patient satisfaction without increasing complications
- Manual soft tissue mobilization combined with conventional physiotherapy leads to better shoulder range of motion and functional outcomes postoperatively
- There is significant variability in postoperative rehabilitation preferences among surgeons, with trauma surgeons generally favoring earlier motion and weight bearing compared to shoulder surgeons
- Early initiation of passive ROM (<2 weeks) is often preferred by trauma surgeons for 2-part fractures, while shoulder surgeons tend to delay passive ROM to 2-6 weeks to protect fixation and tuberosities
- Immobilization duration varies widely but prolonged immobilization can lead to stiffness and frozen shoulder; thus, balancing protection with early mobilization is crucial
- Postoperative protocols must consider patient factors such as comorbidities, fracture pattern, fixation stability, and functional demands to optimize outcomes
Reference:
- Crepaz-Eger, U., Dankl, L., Knierzinger, D., & Hengg, C. (2025). Postoperative treatment of proximal humerus fractures with an early active motion protocol: a prospective randomized controlled trial. Journal of Shoulder and Elbow Surgery, 34(10), 2303-2310. https://doi.org/10.1016/j.jse.2025.01.042
- Fram, B. R., Strony, J. T., Chen, R. E., Namdari, S., & Krieg, J. C. (2024). Proximal humerus fractures: Postoperative protocols and factors affecting treatment decisions among shoulder and elbow and orthopedic trauma surgeons. Journal of Orthopaedics, 49, 75-80. https://doi.org/10.1016/j.jor.2023.11.062
- Patch, D. A., Reed, L. A., Hao, K. A., King, J. J., Kaar, S. G., Horneff, J. G., … Spitler, C. A. (2022). Understanding postoperative rehabilitation preferences in operatively managed proximal humerus fractures: do trauma and shoulder surgeons differ? Journal of Shoulder and Elbow Surgery, 31(5), 1106-1114. https://doi.org/10.1016/j.jse.2021.12.045
- Toteva, L., & Dimitrova, E. (2022). Effectiveness of manual therapy added to conventional physiotherapy protocol in patients with surgically treated proximal humeral fractures. Journal of Applied Sports Sciences, 1, 99-107. https://doi.org/10.37393/JASS.2022.01.9
- Bullock, G. S., Garrigues, G. E., Ledbetter, L., & Kennedy, J. (2019). A systematic review of proposed rehabilitation guidelines following anatomic and reverse shoulder arthroplasty. Journal of Orthopaedic & Sports Physical Therapy, 49(5), 337-346. https://doi.org/10.2519/jospt.2019.8616
- Handoll, H. H. G., & Brorson, S. (2015). Interventions for treating proximal humeral fractures in adults. Cochrane Database of Systematic Reviews, (11), CD000434. https://doi.org/10.1002/14651858.CD000434.pub4