
Overview
Hip fractures are more common in older adults and occur at different rates around the world. In the United States, they are more common in women than men and are expected to increase as the population ages. Most hip fractures in people over 65 happen after a simple fall and are often related to weaker bones (fragility fractures). Although hip fracture rates have declined in some high-income countries due to improved osteoporosis management and fall prevention, rates continue to rise among the very elderly and in low- and middle-income populations.
These fractures are commonly classified as intracapsular or extracapsular. Intracapsular fractures involve the femoral neck, while extracapsular fractures include intertrochanteric and subtrochanteric fractures that occur around or just below the greater trochanter. Surgical management depends on the fracture type and patient-specific factors. Intracapsular fractures may be treated with internal fixation when stable or with hemiarthroplasty or total hip arthroplasty when displaced, with total hip arthroplasty often preferred in younger, more active patients. Extracapsular fractures are typically managed with internal fixation, most commonly using cephalomedullary nails or sliding hip screws, with cephalomedullary nails favored for unstable fracture patterns.
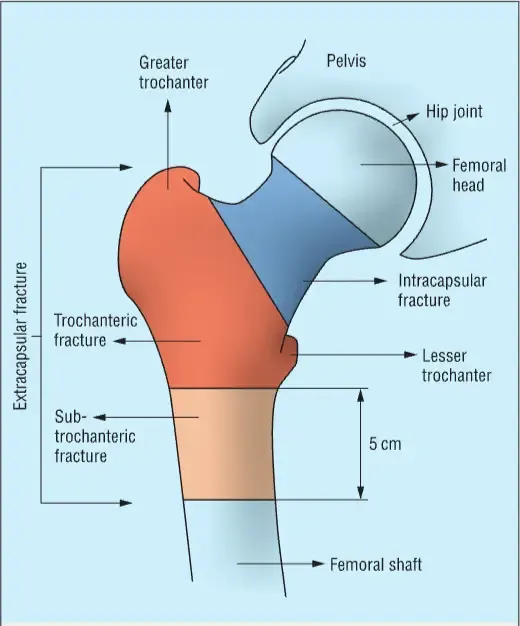
Photo Adapted from McDonough et al. (2021).
Stage 1: Prehabilitation Phase (Pre-Surgery or Immediate Post-Op Day 0-1)
Goals:
- Maintain bronchial hygiene
- Preserve range of motion (ROM) and strength of uninvolved limbs
- Identify and address risk factors for poor rehabilitation outcomes (e.g., cognitive impairment)
- Educate patient and caregivers about postoperative rehabilitation and pain management
Interventions:
- Patient education on surgery and postoperative expectations
- Breathing exercises to prevent pulmonary complications
- Ankle pumps and upper limb exercises to promote circulation and prevent DVT
- Cognitive and emotional support
Suggested Exercises:
- Ankle dorsiflexion and plantarflexion (“ankle pumps”)
- Upper limb ROM exercises
Precautions:
- Avoid excessive movement of fractured hip
- Monitor vital signs and pain
Complications to Monitor:
- Respiratory complications (pneumonia)
- Deep vein thrombosis (DVT)
- Delirium
Weight Bearing:
- Generally non-weight-bearing or toe-touch weight-bearing as per surgical advice
Stage 2: Early Function Phase (Postoperative Day 1 to Hospital Discharge)
Goals:
- Initiate safe mobilization and functional mobility
- Prevent complications related to immobility (pressure ulcers, DVT)
- Begin hip ROM and lower extremity muscle activation
- Educate on safe use of assistive devices and hip precautions
Interventions:
- Initiate early assisted mobilization within 24-48 hours
- Hip joint ROM exercises within pain tolerance
- Isometric quadriceps and gluteal muscle activation
- Balance initiation (seated/standing balance)
- Patient and caregiver education on hip precautions and mobility aids
Suggested Exercises:
- Bed mobility exercises (rolling with pillow support)
- Active hip and knee ROM exercises within pain limits as per surgeon recommendations
- Isometric quadriceps contractions (quad sets)
- Sit-to-stand transfers
- Assisted walking with walker or crutches
Precautions:
- Adhere to surgical team recommendations (based on type of surgery methods)
- Monitor for signs of dislocation, infection, DVT
Complications to Monitor:
- Surgical site infection
- Hip dislocation
- DVT and pulmonary embolism (PE)
- Cognitive decline/delirium
Weight Bearing:
- As tolerated or partial weight bearing depending on fixation stability and surgeon guidance
Stage 3: Progressive Function Phase (Discharge to 6 Weeks Post-Op)
Goals:
- Regain strength and flexibility of operated limb
- Improve balance and proprioception
- Normalize functional mobility (including ADLs)
- Educate on pain coping and safe activity progression
Interventions:
- Progressive resistance exercises (PRE) targeting hip abductors, hip & knee extensors
- Balance and proprioceptive training
- Gait training emphasizing normalized patterns
- Begin endurance training (e.g., treadmill walking, stationary cycling)
- Continue patient and caregiver education on activity progression and fall prevention
Suggested Exercises:
- Progressive resistance training: knee extensions, hip abduction & flexion
- Balance exercises: single-leg stance (unaffected side), weight shifts, tandem walking
- Gait training with assistive device as needed
- Stair climbing practice
Precautions:
- Continue hip precautions as per surgical approach
- Avoid high-impact or excessive loading activities
- Monitor for signs of implant loosening or fracture nonunion
Complications to Monitor:
- Implant-related complications (loosening, dislocation)
- Post-traumatic arthritis signs
- Muscle atrophy or weakness
Weight Bearing:
- Progress to full weight-bearing as tolerated, guided by clinical and radiographic healing
- For ORIF: partial to full weight-bearing progression generally over 6-12 weeks
- For arthroplasty:
Cemented implants: Immediate full weight-bearing often permitted
Non-cemented implants: may require modified or protected weight-bearing for several weeks to allow osseointegration, depending on surgeon protocol and bone quality
Stage 4: Advanced Function Phase (7 to 12 Weeks Post-Op and Beyond)
Goals:
- Achieve pre-fracture functional status or as close as possible
- Improve lower extremity strength, endurance, and aerobic capacity
- Return to work, community, and recreational activities
- Relax some hip precautions if clinically appropriate
Interventions:
- Continued progressive resistance and endurance training
- Community ambulation training, including uneven terrain and outdoor walking
- Aerobic conditioning (cycling, swimming)
- Functional and occupational therapy targeting ADLs and instrumental ADLs (IADLs)
- Psychological support and motivational interviewing if indicated
Suggested Exercises:
- Advanced balance activities (dynamic balance, obstacle negotiation)
- Aerobic exercise (stationary bike, treadmill)
- Functional task practice (stairs, shopping simulation)
- Resistance training with increased intensity
Precautions:
- Relax hip precautions cautiously, based on surgical approach, implant stability, and clinical judgment
- Monitor for overuse injuries or falls
Complications to Monitor:
- Late implant complications (loosening, wear)
- Persistent pain or functional decline
Weight Bearing:
- Full weight-bearing generally allowed
- Patient encouraged to progressively increase activity levels
Additional Considerations Across All Phases:
- Multidisciplinary Approach: Integral for optimal outcomes including orthopedics, physiotherapy, occupational therapy, nursing, nutrition, and geriatric medicine
- Nutritional Support: Early assessment and intervention with protein supplementation, vitamin D, and calcium to enhance healing and functional recovery
- Venous Thromboembolism (VTE) Prevention: Pharmacologic and mechanical prophylaxis recommended, along with early mobilization
- Pain Management: Use of peripheral nerve blocks (e.g., femoral nerve block) effective to control pain and facilitate rehabilitation
- Cognitive and Psychological Support: Addressing fear of falling and depression is important for rehabilitation success
- Compliance Monitoring: Use of biofeedback and wearable sensors is encouraged to improve adherence to weight-bearing and exercise protocols
- Home-Based and Community Rehabilitation: Effective as continuation of inpatient rehab to promote long-term recovery and community reintegration
Summary Table of Postoperative Rehabilitation Protocol for Hip Fracture
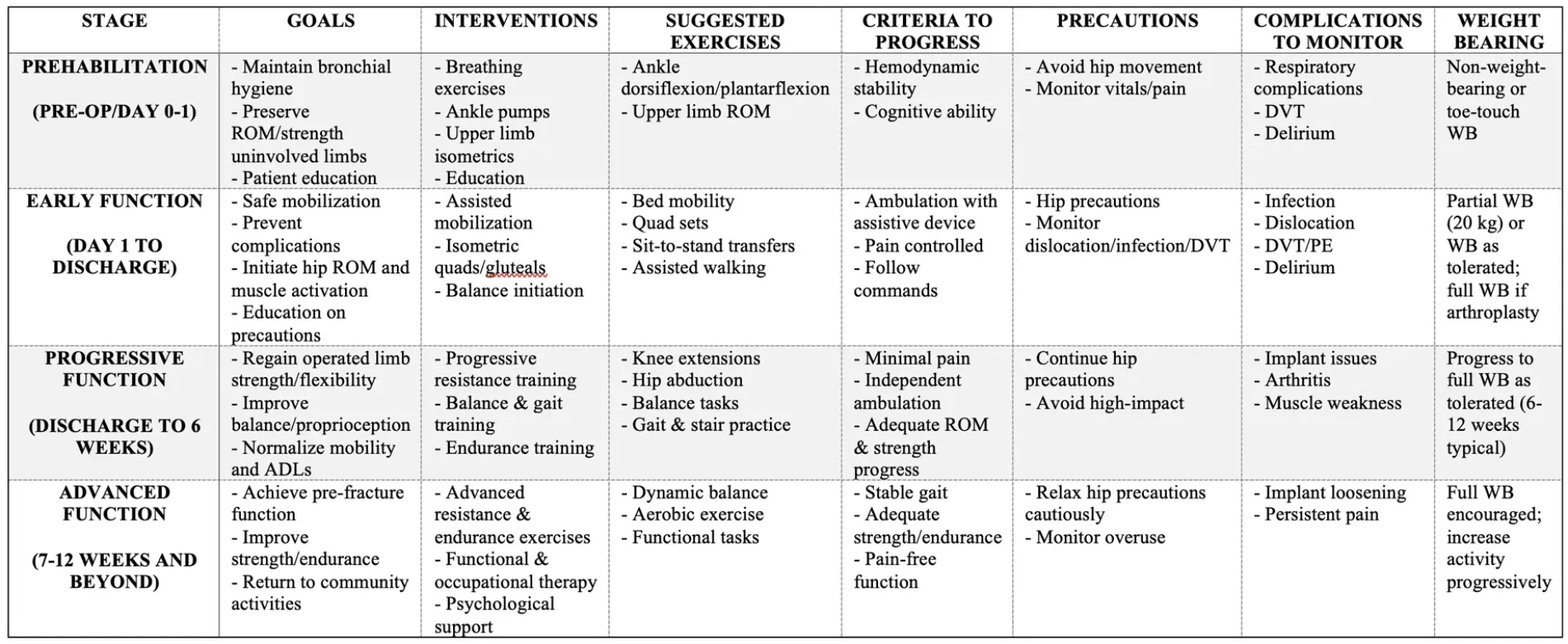
Important Points and Updates from the Literature
- Weight-Bearing Protocols: There is considerable variability and lack of consensus. ORIF patients often require partial or restricted weight-bearing for 6-12 weeks, while arthroplasty patients may have immediate full weight-bearing
- Early Mobilization: Initiating mobilization within 24-48 hours post-surgery improves functional outcomes, reduces hospital stay, and lowers mortality
- Multidisciplinary Care: Involving geriatricians, physiatrists, nutritionists, and therapists improves functional recovery, reduces complications, and is cost-effective
- Nutritional Support: Protein supplementation and vitamin D/calcium improve functional outcomes and reduce complications
- Pain Management: Peripheral nerve blocks are effective in reducing pain and delirium, facilitating rehabilitation
- Home-Based Rehabilitation: Effective continuation of inpatient care, though evidence is mixed regarding superiority over hospital-based rehab
- Cognitive and Psychological Factors: Fear of falling and cognitive impairment affect rehabilitation success; psychological interventions like motivational interviewing show promise but need further evidence
- Compliance Monitoring: Technologies like biofeedback insoles can improve adherence to weight-bearing restrictions
- Long-Term Outcomes: Rehabilitation improves physical and social community reintegration; however, psychological and home-based intervention effects require further study
Reference:
- Sing, C. W., Lin, T. C., Bartholomew, S., Bell, J. S., Bennett, C., Beyene, K., … & Wong, I. C. (2023). Global epidemiology of hip fractures: secular trends in incidence rate, post‐fracture treatment, and all‐cause mortality. Journal of Bone and Mineral Research, 38(8), 1064-1075. https://doi.org/10.1002/jbmr.4821
- Ivanova, S., Prochazka, O., Giannoudis, P. V., Tosounidis, T., Tannast, M., & Bastian, J. D. (2025). Rehabilitation protocols for surgically treated acetabular fractures in older adults: Current practices and outcomes. Journal of Clinical Medicine, 14(4912). https://doi.org/10.3390/jcm14144912
- Koudouna, S., Evangelopoulos, D. S., Sarantis, M., Chronopoulos, E., Dontas, I. A., & Pneumaticos, S. (2023). The effect of postoperative physical therapy following hip fracture: A literature review. Cureus, 15(4), e37676. https://doi.org/10.7759/cureus.37676
- Lee, K.-J., Um, S.-H., & Kim, Y.-H. (2020). Postoperative rehabilitation after hip fracture: A literature review. Hip & Pelvis, 32(3), 125-131. https://doi.org/10.5371/hp.2020.32.3.125
- Lizano-Diez, X., Johann Baptist Keel, M., Siebenrock, K. A., Tey, M., & Bastian, J. D. (2020). Rehabilitation protocols in unstable trochanteric fractures treated with cephalomedullary nails in elderly: current practices and outcome. European Journal of Trauma and Emergency Surgery, 46(6), 1267-1280. https://doi.org/10.1007/s00068-019-01294-z
- McDonough, C. M., Harris-Hayes, M., Kristensen, M. T., Overgaard, J. A., Herring, T. B., Kenny, A. M., & Mangione, K. K. (2021). Physical therapy management of older adults with hip fracture: Clinical practice guidelines linked to the international classification of functioning, disability and health. Journal of Orthopaedic & Sports Physical Therapy, 51(2), CPG1-CPG81. https://doi.org/10.2519/jospt.2021.0301
- Min, K., Beom, J., Kim, B. R., Lee, S. Y., & Lim, J. Y. (2021). Clinical practice guideline for postoperative rehabilitation in older patients with hip fractures. Annals of Rehabilitation Medicine, 45(3), 225-259. https://doi.org/10.5535/arm.21110
- Nandini, V., Mohanan, C., Peter, A. L. A., Jeldi, A. J., Sameer, M., & Kannan, S. (2025). Structured exercise program for hip arthroplasty: An expert consensus using the Delphi technique. Indian Journal of Orthopaedics, 59(3), 539-548. https://doi.org/10.1007/s43465-025-01335-3
- Phang, J. K., Lim, Z. Y., Yee, W. Q., Tan, C. Y. F., Kwan, Y. H., & Low, L. L. (2023). Post-surgery interventions for hip fracture: A systematic review of randomized controlled trials. BMC Musculoskeletal Disorders, 24, 417. https://doi.org/10.1186/s12891-023-06512-9
- Storr, B., Peiris, C. L., & Snowdon, D. A. (2022). Community reintegration after rehabilitation for hip fracture: A systematic review and meta-analysis. Archives of Physical Medicine and Rehabilitation, 103(9), 1638-1650. https://doi.org/10.1016/j.apmr.2021.12.007

