Overview
Rehabilitation after ATSA aims to protect healing tissues (especially the subscapularis), restore range of motion (ROM), regain strength, and return patients to functional activities while minimizing complications. The protocol is generally divided into three phases spanning approximately the first 6 months postoperatively, with continued maintenance thereafter.
Phase 1: Immediate Postoperative Phase (Postoperative Day 1 to Week 6)
Goals
- Protect the healing subscapularis tendon, joint capsule, and biceps tenodesis.
- Control pain and swelling.
- Maintain distal circulation and mobility (elbow, wrist, hand).
- Prevent stiffness without compromising repair.
- Educate patient on precautions and safe use of the arm.
- Ensure proper sling use and fit.
Precautions
- Use of sling with abduction pillow continuously (day and night) for 4-6 weeks to protect the subscapularis repair. Avoid hand behind back and external rotation (ER) at 90° abduction.
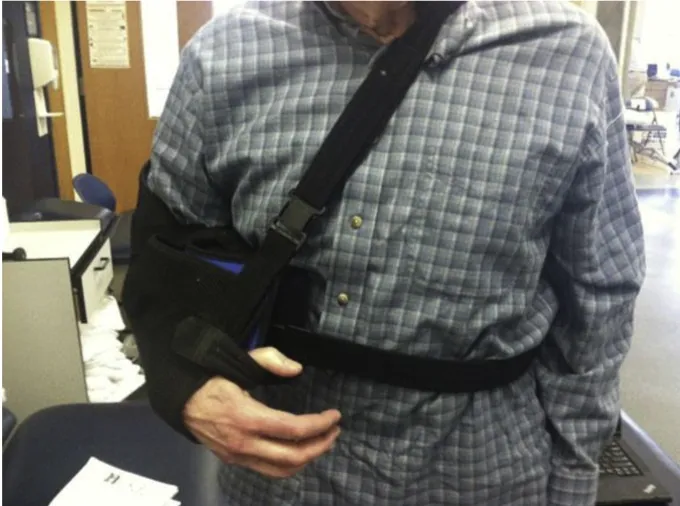
Adapted from Kennedy et al., 2020
- No active shoulder elevation.
- No weight bearing through the operative arm.
- No submersion of the shoulder in water until incision healing (~4 weeks).
- Limit ER to 20°-30° with arm at side depending on subscapularis takedown technique (lesser tuberosity osteotomy (LTO) allows up to 30°, tenotomy or peel more conservative at 20°).
- Avoid internal rotation (IR) behind the back or into hip pocket and resisted IR at least for 6 weeks
- Avoid activities that place strain on the subscapularis repair.
- While in supine, support arm on pillow to avoid GH extension past neutral.
- Light ADL permitted with elbow at waist level (eating, writing)
Interventions & Exercises
- Passive Range of Motion (PROM): Begin gentle PROM within safe limits (e.g., forward flexion (FF) up to 120°, ER 0°-30°, avoid ER at 90° abduction).
- Distal joint mobility: Active ROM (AROM) of elbow, wrist, and hand.
- Pendulum exercises: Gentle Codman pendulums to promote joint fluid circulation.
- Scapular retraction and depression: To optimize glenoid position.
- Patient education: Sling management, activity restrictions, precautions.
Criteria to Progress to Phase 2
- Pain controlled (less than 3/10 at rest).
- Healing incision without signs of infection.
- Ability to don/doff sling properly.
- Achieving PROM goals (FF to ~120°, ER to ~30° at side).
- Surgeon clearance, typically after 4-6 weeks post-op radiograph assessment.
Limitations
- Avoid active shoulder elevation and resisted IR.
- Strict sling use required.
- No lifting or weight bearing with operative arm.
- Avoid submersion of operated shoulder.
Phase 2: Intermediate Phase (Weeks 7 to 12)
Goals
- Gradually restore mobility without compromising repair.
- Begin active assisted range of motion (AAROM), progressing to active ROM (AROM).
- Begin gentle functional IR.
- Initiate light isometric strengthening avoiding closed-chain exercises.
- Gentle stretching after 6-8 weeks
- Continue pain management and swelling control.
- Increase use of arm in activities of daily living (ADL) gradually.
Precautions
- Discontinue sling use at 4-6 weeks (surgeon dependent).
- Limit ER in scapular plane to 60°.
- No GH extension past neutral (up to 6 weeks)
- Delay resisted rotation for several weeks
- Avoid closed-chain and weight-bearing exercises.
- Progress IR behind back gradually, typically limited to sacrum or lumbar spine level.
Interventions & Exercises
- PROM, AAROM, AROM: Progress PROM beyond Phase 1 limits; begin AAROM and AROM in all planes within safe limits.
- Active elevation progression: From supine to upright positions with short to long lever arm (bent to straight elbow) to gradually increase deltoid and rotator cuff activation.
- Isometric strengthening: Deltoid, rotator cuff, scapular muscles; avoid resistance that stresses subscapularis.
- Functional activities: Begin light ADLs with arm use while avoiding heavy lifting (limit to 3 lb)
- Aerobic activities: Low impact (walking, stationary bike).
- Scapular stabilization and rhythmic stabilization exercises.
Criteria to Progress to Phase 3
- Achieve PROM and AROM goals appropriate for the patient’s diagnosis (e.g., 140°-150° forward elevation for osteoarthritis patients).
- No pain or signs of inflammation with increased activity.
- Functional use of arm in ADLs without compensation.
- Surgeon and therapist approval.
Limitations
- Avoid heavy resistance and impact loading.
- No weight bearing or closed-chain exercises.
- Limit ER beyond 60° and IR behind back cautiously.
Phase 3: Advanced Strengthening and Return to Function (Week 12+)
Goals
- Achieve full painless ROM.
- Improve muscle strength and endurance.
- Restore functional use of the arm for work, sport, and recreational activities.
- Promote return to prior activity levels while protecting the repair.
Precautions
- Avoid heavy lifting above shoulder level or anterior to frontal plane.
- Avoid impact or high-stress activities (e.g., wood chopping, bench pressing) until after 6 months.
- Gradual return to sports starting around 4 months; full return usually not before 6 months.
Interventions & Exercises
- Strengthening: Progressive resistance training including rotator cuff, deltoid, periscapular muscles using bands, light weights, gym machines.
- Closed-chain exercises: Planks, yoga, quadruped exercises as tolerated.
- Functional training: Sport-specific drills, work-related tasks.
- Aerobic conditioning: Swimming, jogging, cycling as tolerated.
- Stretching: Continue gentle stretching to maintain mobility.
Criteria for Discharge or Maintenance Phase
- Pain-free use of shoulder in ADLs and recreational activities.
- Achieved functional goals specific to patient.
- Satisfactory muscle strength and joint stability.
- Patient confidence and ability to self-manage exercises.
Limitations
- Avoid heavy impact or high load activities until full healing.
- Monitor for any signs of instability or pain.
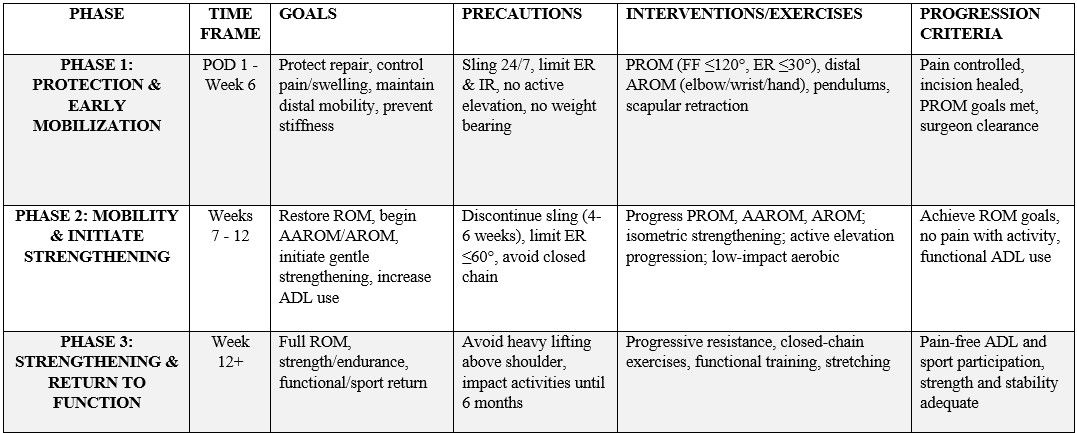
Summary Table: Postoperative Rehabilitation Stages Following ATSA
Additional Points & Interesting Tips
- Sling Position Matters: A neutral rotation sling with an abduction pillow reduces night pain and improves ROM better than an internal rotation sling during Phase 1.
- Subscapularis Healing: Management technique (tenotomy, peel, or LTO) influences the safe range of ER and progression pace; communication with surgeon is essential.
- Immediate vs Delayed Mobilization: Early passive and active-assisted ROM may improve function and reduce pain in the early postoperative period but shows no long-term difference.
- Tele-rehabilitation Viability: Telerehabilitation yields comparable ROM and patient-reported outcomes to in-person physical therapy, offering convenience without compromising recovery.
- Variability in Protocols Online: There is significant variation in rehabilitation protocols across institutions, often diverging from consensus guidelines, highlighting the need for tailored, evidence-based approaches.
- Patient Education & Expectations: Prehabilitation and clear education about restrictions, progression, and expected timelines can improve patient satisfaction and adherence.
- Strengthening Progression: Start with isometric exercises and progress to resistance training below shoulder level and anterior to the frontal plane to protect healing tissues.
- Neutral Rotation Sling Position: The study found moderate evidence that using a neutral rotation sling position (sling with an abduction cushion) after anatomic total shoulder arthroplasty results in less night pain and greater range of motion, especially in external rotation, compared to an internal rotation sling position. This finding has practical implications for post-operative rehabilitation protocols.
- Modifiable vs Non-modifiable Factors: The review differentiates between modifiable factors (e.g., physical therapy protocols, sling position, immediate range of motion exercises, telemedicine) and non-modifiable factors (e.g., gender, implant type, soft tissue integrity of the rotator cuff). Most factors had only preliminary or conflicting evidence regarding their association with better treatment outcomes, highlighting the complexity of rehabilitation after shoulder arthroplasty.
- Pre-operative Function and Range of Motion: Pre-operative shoulder function and range of motion are associated with post-operative improvements, where patients with lower pre-operative function or range of motion showed larger gains post-operatively, which is consistent with findings in other orthopedic conditions.
- Heterogeneity and Need for Standardization: A major limitation highlighted is the heterogeneity in physical therapy protocols, implant types, outcome measures, and follow-up times across studies, which complicates drawing firm conclusions. The authors emphasize the need for more high-quality research with standardized protocols to better determine factors influencing rehabilitation outcomes.
Reference:
Claes, A., Mertens, M. G. C. A. M., Verborgt, O., Baert, I., & Struyf, F. (2022). Factors associated with better treatment outcome of physical therapy interventions after shoulder arthroplasty: A systematic review. Clinical Rehabilitation, 36(10), 1369-1399. https://doi.org/10.1177/02692155221106627
Denard, P. J., & Lädermann, A. (2016). Immediate versus delayed passive range of motion following total shoulder arthroplasty. Journal of Shoulder and Elbow Surgery, 25(12), 1918-1924. https://doi.org/10.1016/j.jse.2016.07.032
Edwards, P. K., Ebert, J. R., Littlewood, C., Ackland, T., & Wang, A. (2020). A randomized trial comparing two rehabilitation approaches following reverse total shoulder arthroplasty. Shoulder & Elbow. https://doi.org/10.1177/1758573220937394
Kennedy, J. S., Garrigues, G. E., Pozzi, F., Zens, M. J., Gaunt, B., Phillips, B., et al. (2020). The American Society of Shoulder and Elbow Therapists’ consensus statement on rehabilitation for anatomic total shoulder arthroplasty. Journal of Shoulder and Elbow Surgery, 29(10), 2149-2162. https://doi.org/10.1016/j.jse.2020.05.019
Mehta, N., Acuna, A. J., McCormick, J. R., et al. (2024). Publicly available anatomic total shoulder arthroplasty rehabilitation protocols show high variability and frequent divergence from the 2020 ASSET recommendations. International Journal of Sports Physical Therapy, 19(7), 856-867. https://doi.org/10.26603/001c.118926
Moffatt, M., Whelan, G., Gill, P., Mazuquin, B., Edwards, P., Peach, C., et al. (2022). Effectiveness of early versus delayed rehabilitation following total shoulder replacement: A systematic review. Clinical Rehabilitation, 36(2), 190-203. https://doi.org/10.1177/02692155211044137
O’Reilly, O. C., Bozoghlian, M., Glass, N., Shaffer, M., Fleming, J., Nepola, J. V., & Patterson, B. M. (2025). Physical therapy following shoulder arthroplasty: an assessment of telerehabilitation vs. in-person physical therapy. Seminars in Arthroplasty, 35(4), 505-516. https://doi.org/10.1053/j.sart.2025.04.009
Schick, S., Dombrowsky, A., Egbaria, J., Paul, K. D., Brabston, E., Momaya, A., & Ponce, B. (2023). Variability in physical therapy protocols following total shoulder arthroplasty. Clinics in Shoulder and Elbow, 26(3), 267-275. https://doi.org/10.5397/cise.2023.00115