Reverse shoulder arthroplasty (RSA) is a surgical procedure in which the normal ball-and-socket anatomy of the shoulder is reversed, placing the ball on the glenoid and the socket on the humerus. This design allows the deltoid muscle to compensate for deficient or torn rotator cuff musculature, restoring shoulder elevation and function. RSA is commonly indicated for cuff tear arthropathy, complex fractures, or failed prior shoulder surgeries. The following is a sample of a comprehensive rehabilitation protocol following this surgery.
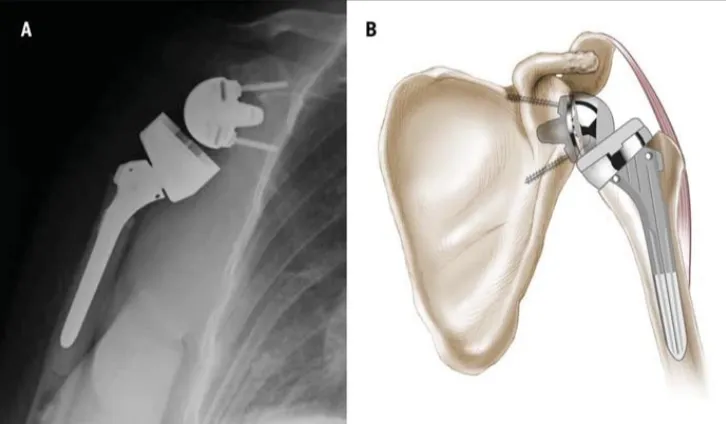
Photo adapted from Boudreau et al., 2007
Phase I: Immediate Post-Surgical / Joint Protection Phase (Day 1 to Week 6)
Goals:
- Protect the surgical repair and ensure healing of soft tissues.
- Maintain joint integrity.
- Control pain and inflammation.
- Maintain mobility and function of distal joints (elbow, wrist, hand).
- Begin gentle passive range of motion (PROM) within safe limits.
Precautions:
- Wear an abduction sling for comfort and protection (typically 4-6 weeks); can be discontinued earlier based on surgeon’s advice and patient tolerance. For the first 2-3 weeks post-operatively, the sling is typically worn full-time and removed only for hygiene, gentle exercises, and therapy sessions, in accordance with the surgeon’s recommendations.
- Avoid shoulder extension and IR beyond neutral.
- No active shoulder range of motion (AROM).
- Only light, NWB isometrics of scapular stabilizers and deltoid
- No lifting or weightbearing through the operated arm.
- Avoid combined shoulder internal rotation (IR), adduction, and extension (e.g., no reaching behind back or pushing from a chair) for at least the first 6 weeks.
- Protect the subscapularis repair if present; if repaired via superior approach, delay PROM and deltoid isometrics for 3-4 weeks.
Interventions:
- Cryotherapy for pain and swelling control.
- PROM of shoulder in scapular plane: forward flexion and external rotation gradually increased up to 90° and 20-30° respectively, avoiding abduction initially.
- Active and active-assisted ROM (AAROM) of elbow, wrist, and hand.
- Submaximal, pain-free deltoid and periscapular isometrics starting around day 4-7 (avoiding shoulder extension during posterior deltoid activation).
- Pendulum exercises.
- Patient and caregiver education on joint protection and safe movement.
List of Exercises:
- Pendulum exercises.
- Passive forward flexion and external rotation in scapular plane (in supine).
- Active elbow/wrist/hand movements.
- Submaximal deltoid isometrics (without shoulder extension).
- Scapular isometrics.
Criteria to Progress to Phase II:
- Patient tolerates PROM and AROM program for elbow, wrist, and hand.
- Ability to isometrically activate all deltoid components and periscapular muscles without pain.
- No signs of instability or complications.
Phase II: Active Range of Motion (AROM) and Early Strengthening Phase (Weeks 6 to 12)
Goals:
- Gradually restore active shoulder ROM.
- Re-establish dynamic shoulder stability.
- Begin gentle strengthening exercises.
- Submaximal isometric exercises (NWB only)
- Continue pain and inflammation control.
- Maintain joint protection.
Precautions:
- Continue avoiding shoulder hyperextension.
- Restrict lifting heavier than a coffee cup.
- Avoid weightbearing with the operative arm.
- If subscapularis repair was done, limit ER and IR as per surgeon’s instructions.
- Avoid sudden or jerky movements to minimize risk of dislocation
Interventions:
- Progress PROM to AAROM and then AROM in scapular plane (supine progressing to sitting/standing).
- Initiate gentle submaximal isometric external and internal rotation.
- Begin gentle isotonic strengthening of deltoid and periscapular muscles with low load, high repetition.
- Gentle scapulothoracic rhythmic stabilization and alternating isometric exercises.
- Continue cryotherapy as needed.
- Functional activities such as feeding and light ADLs encouraged.
- Restricted lifting with operated arm for 12-16 weeks (no more than a cup of coffee or glass of water)
- Delay resisted rotation to protect subscapularis and teres minor
List of Exercises:
- Pulley-assisted forward flexion.
- Assisted wall slides.
- Active forward flexion (gravity minimized progressing to upright).
- Submaximal ER strengthening in 45° to 90° abduction.
- Isometric deltoid and scapular stabilizer contractions.
- Gentle scapular retractions and protractions.
- Elbow, wrist, and hand strengthening.
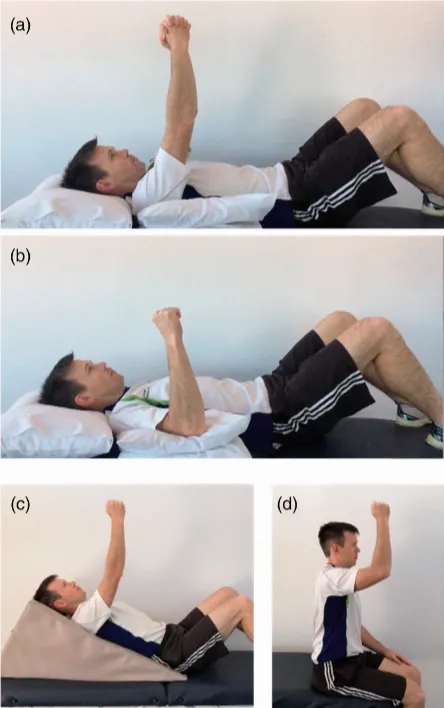
Progressive active forward flexion exercises, starting
with (a) supine ‘pray and lift’; (b) supine forward flexion; (c)
incline forward flexion; (d) upright forward flexion
Photo adapted from Edwards et al., 2021
Criteria to Progress to Phase III:
- Demonstrated improved shoulder function.
- Ability to isotonically activate all deltoid and periscapular muscles.
- Pain-free AROM with acceptable mechanics.
Phase III: Moderate Strengthening Phase (Week 12 and Beyond)
Goals:
- Enhance functional use of the shoulder.
- Increase muscular strength, endurance, and power.
- Normalize shoulder mechanics.
- Prepare for return to higher-level activities.
Precautions:
- Avoid lifting objects heavier than 2.7 kg (6 lbs).
- No sudden lifting, pushing, or jerking motions.
- Continue joint protection strategies as needed.
Interventions:
- Progressive resisted strengthening of deltoid, rotator cuff, and scapular stabilizers using weights and resistance bands.
- Initiate eccentric and plyometric exercises around 12 weeks.
- Closed chain exercises for proprioception.
- Functional activity simulation and task-oriented exercises.
List of Exercises:
- Supine to standing active forward flexion with light weights.
- Resisted external and internal rotation exercises with therabands or dumbbells.
- Scapular setting exercises progressing to rows and scapular stabilization drills.
- Eccentric strengthening exercises.
- Closed chain proprioceptive exercises.
Criteria to Progress to Phase IV:
- Independent with home exercise program.
- Demonstrates functional pain-free AROM (80°-120° elevation, ~30° ER).
- Sufficient strength and control to perform ADLs safely.
Phase IV: Continued Home Program (Typically 4+ Months Postoperative)
Goals:
- Maintain strength, endurance, and ROM.
- Return to functional and recreational activities within surgeon’s guidelines.
- Prevent complications and overuse injuries.
Precautions:
- Continue lifting restrictions as advised.
- Avoid high-risk activities unless cleared by surgeon/therapist.
Interventions:
- Patient-directed home exercise focusing on continued strengthening and ROM.
- Gradual return to work, sports, and leisure activities.
- Periodic follow-up monitoring.
List of Exercises:
- Continued resistance exercises for deltoid and scapular muscles.
- Stretching and mobility exercises as needed.
- Functional task practice.
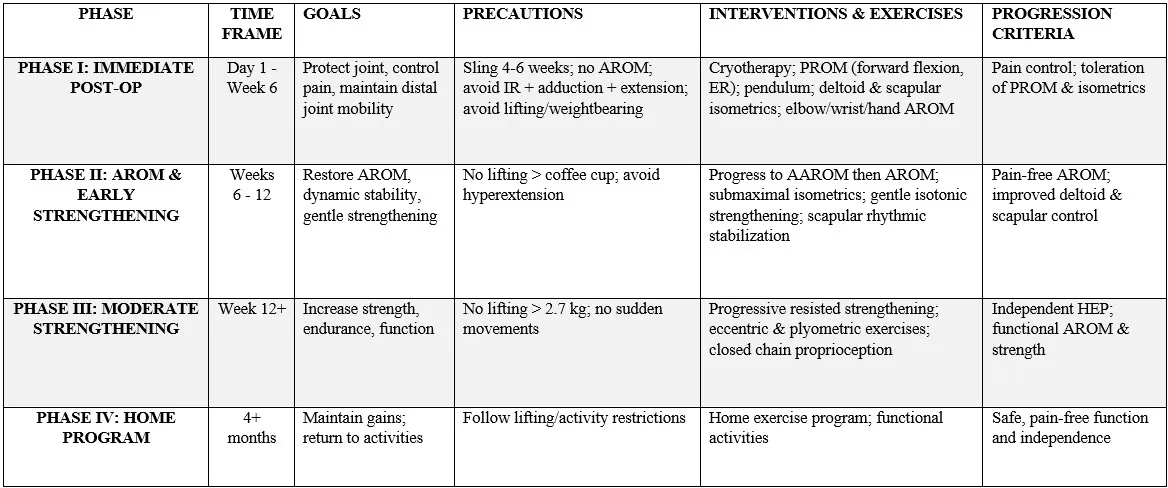
Summary Table of Rehabilitation Protocol
Additional Key Points and Tips
- Sling Position Matters: Neutral rotation sling position has been shown to reduce night pain and improve range of motion compared to internal rotation slings, especially in anatomic TSA patients.
- Early Mobilization is Safe: Multiple studies demonstrate that early initiation of passive and active exercises does not increase complication rates, and can improve early function.
- Subscapularis Repair Considerations: When subscapularis is repaired, delayed initiation of ER and IR ROM and strengthening is recommended to protect repair; however, many modern RTSA procedures do not repair subscapularis and allow earlier mobilization.
- Home-based vs. Supervised Therapy: Home exercise programs can be as effective as formal supervised therapy in most patients, reducing costs and patient burden.
- Return to Sport and Activities: Most elderly patients can safely return to low- and moderate-impact sports post-RTSA; however, higher demand activities should be individualized and cautiously approached.
- Deltoid Muscle Focus: Given the altered biomechanics after RTSA, deltoid muscle strengthening is critical for functional recovery. Use biofeedback and progressive loading to optimize deltoid recruitment.
References
- Boudreau, S., Boudreau, E. D., Higgins, L. D., & Wilcox, R. B. (2007). Rehabilitation following reverse total shoulder arthroplasty. Journal of Orthopaedic & Sports Physical Therapy, 37(12), 734-743.
- Claes, A., Mertens, M. G. C. A. M., Verborgt, O., Baert, I., & Struyf, F. (2022). Factors associated with better treatment outcome of physical therapy interventions after shoulder arthroplasty: A systematic review. Clinical Rehabilitation, 36(10), 1369-1399.
- Edwards, P. K., Ebert, J. R., Joss, B., Ackland, T., & Wang, A. (2021). A randomised trial comparing two rehabilitation approaches following reverse total shoulder arthroplasty. Shoulder & Elbow, 13(5), 557-572.
- Hagen, M. S., Allahabadi, S., Zhang, A. L., Feeley, B. T., Grace, T., & Ma, C. B. (2020). A randomized single-blinded trial of early rehabilitation versus immobilization after reverse total shoulder arthroplasty. Journal of Shoulder and Elbow Surgery, 29(3), 442-450.
- Lee, J., Consigliere, P., Fawzy, E., et al. (2021). Accelerated rehabilitation following reverse total shoulder arthroplasty. Journal of Shoulder and Elbow Surgery, 30(9), e545-e557.
- Sachinis, N. P., Yiannakopoulos, C. K., Berthold, D. P., Franz, A., & Beitzel, K. (2024). Can we accelerate rehabilitation following reverse shoulder arthroplasty? A systematic review. Shoulder & Elbow, 16(2), 214-227.
- Schick, S., Elphingstone, J., Paul, K., et al. (2023). Home-based physical therapy results in similar outcomes to formal outpatient physical therapy after reverse total shoulder arthroplasty: a randomized controlled trial. Journal of Shoulder and Elbow Surgery, 32(8), 1555-1561.
- Bardsley, J. L., Daw, R. L. C., Gibson, J., et al. (2024). Physiotherapy treatment for reverse total shoulder arthroplasty: Results of a patient-centred rehabilitation guideline using functional and patient-reported outcome measures. Shoulder & Elbow, 16(3), 330-335.