Introduction
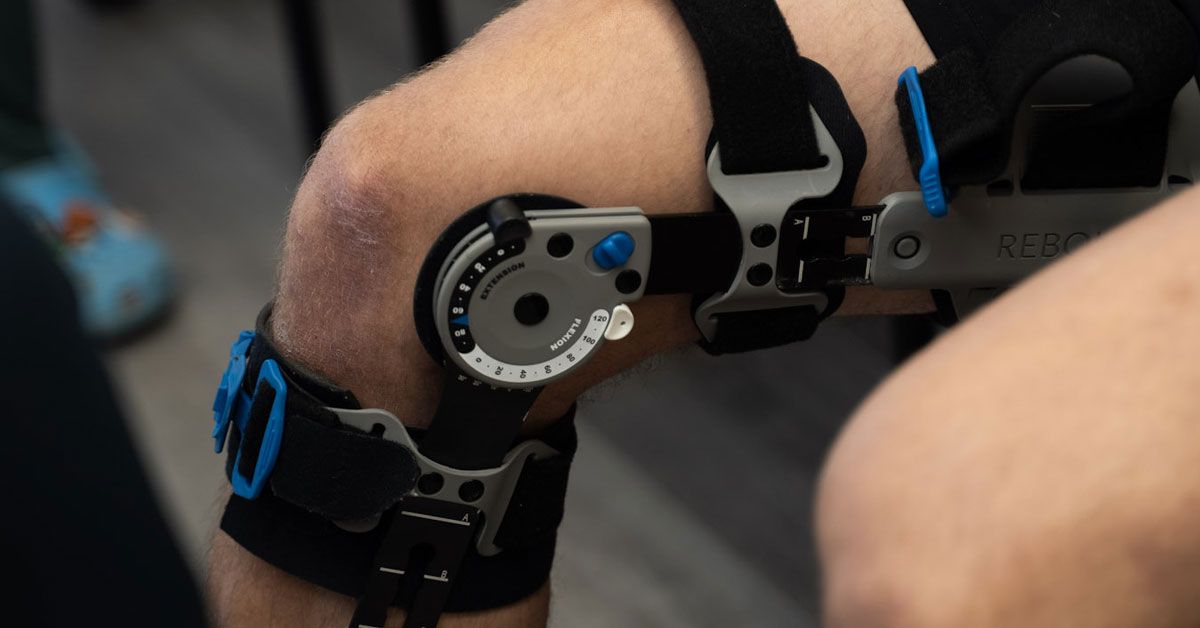
Total Knee Arthroplasty (TKA) is a common surgical intervention for end-stage osteoarthritis, aimed at reducing pain and restoring function. Postoperative rehabilitation is essential to optimize outcomes including pain relief, restoration of range of motion (ROM), muscle strength, physical function, and quality of life. Rehabilitation after TKA is a complex, multifactorial intervention involving various components such as strengthening, flexibility, balance, education, and adjunctive modalities, delivered across different phases post-surgery. Despite diverse protocols, the literature suggests comparable improvements across rehabilitation programs when key elements are addressed. This synthesis integrates evidence and recommendations from six comprehensive papers to provide a clear, practical rehabilitation guideline for physiotherapy practice.
Stage 1: Immediate Postoperative Phase (Day 0 to Day 3)
Goals
- Control pain and inflammation
- Prevent complications (e.g., deep vein thrombosis, infection)
- Initiate early mobilization and functional activities (sitting, standing, walking with aids)
- Restore knee range of motion (ROM) gradually
- Begin muscle activation, especially quadriceps
Precautions
- Monitor pain levels closely; keep pain manageable (NRS scores below 4 recommended)
- Avoid excessive swelling; control edema with proper positioning and cryotherapy
- Observe for signs of complications (dizziness, orthostatic hypotension, wound issues)
- Avoid unsupported walking and high-risk activities until sufficient strength and control are achieved
- Use assistive devices as recommended
Interventions
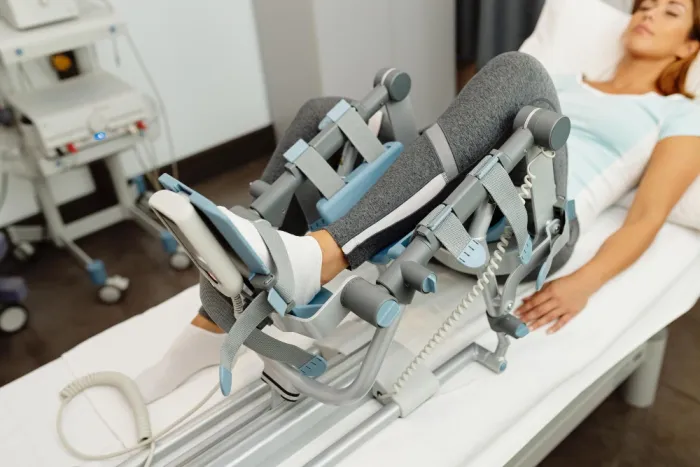
- Continuous Passive Motion (CPM) can be used briefly (~1 hour/day) within the first 24 hours but is not recommended as standard care due to lack of evidence for long-term benefits.
- Cryotherapy application to reduce pain and swelling; educate patient and caregivers on safe use.
- Compression bandaging and suction drainage management.
- Early mobilization: sitting, active ankle pumps, isometric quadriceps and gluteal sets, active-assisted knee flexion/extension within pain tolerance.
- Assisted standing and walking with walker or crutches initiated by Day 2-3.
- Patient education on safe transfers, use of assistive devices, and fall prevention.
Exercises
- Ankle pumps (to prevent venous stasis)
- Quadriceps setting (isometric contraction with knee extended)
- Gluteal sets
- Heel slides (active-assisted knee flexion)
- Assisted knee extension
- Bed mobility exercises (rolling, scooting, supine to sitting)
- Sit to stand with assistance
- Gait training with assistive devices
Important Points
- Early rehabilitation within 24 hours shortens hospital stay and improves outcomes.
- Pain control is essential to facilitate participation in therapy.
- Knee positioning during rest in mild flexion (30°-90°) can reduce postoperative swelling and blood loss without compromising long-term ROM.
- Monitor for and manage adverse effects such as dizziness and orthostatic hypotension.
Stage 2: Acute Rehabilitation Phase (Week 1 to Week 4)
Goals
- Increase active knee ROM aiming for functional range (ideally 0° extension to ~110° flexion)
- Improve quadriceps and lower limb muscle strength
- Enhance functional mobility: transfers, walking, stair climbing
- Begin balance and proprioceptive training
- Continue pain and swelling management
Precautions
- Avoid overstressing the joint or surgical wound
- Progress exercises based on patient tolerance and clinical assessment
- Be vigilant for signs of complications or adverse responses
- Use proper gait mechanics to avoid compensations
Interventions
- Progressive strengthening exercises targeting quadriceps, hamstrings, hip abductors, and adductors.
- Task-specific training including sit-to-stand, step-ups/downs, walking practice.
- Balance and motor learning exercises (e.g., single-leg stance, weight shifts, tandem walking).
- Adjunctive modalities if indicated: neuromuscular electrical stimulation (NMES) to improve quadriceps activation, biofeedback, and possibly transcutaneous electrical nerve stimulation (TENS) for pain.
- Aerobic conditioning as tolerated (e.g., stationary cycling, walking) introduced gradually.
- Patient education focusing on activity modification, pain management, and home exercise adherence.
Exercises
- Straight leg raises
- Short arc quads
- Knee extension/flexion strengthening
- Hip abduction/adduction exercises
- Step-ups and step-downs
- Sit-to-stand repetitions
- Balance exercises (single leg stance, weight shifts)
- Stationary cycling or aquatic therapy (if available)
- Gait training with focus on symmetry and proper mechanics
Important Points
- High-intensity strength training initiated early (within first week) is safe and improves strength and function.
- NMES is beneficial especially in patients with quadriceps activation deficits.
- Early gait training and task-specific functional training improve outcomes.
- Balance training reduces fall risk and improves mobility.
- Progression should be individualized, using patient response to guide intensity and volume.
Stage 3: Post-Acute Rehabilitation Phase (Week 5 to Month 3)
Goals
- Restore full functional ROM (aim for >120° flexion)
- Maximize strength and endurance of lower extremity muscles
- Improve balance, proprioception, and motor control
- Enhance endurance and aerobic capacity
- Facilitate return to activities of daily living (ADLs), work, and recreational activities
- Promote patient self-management and adherence to home exercise program
Precautions
- Avoid overuse injuries; monitor for pain or swelling post-exercise
- Consider patient comorbidities and surgical factors when progressing
- Continue to watch for signs of joint stiffness or arthrofibrosis
Interventions
- Continued progressive resistive strengthening exercises targeting lower limb musculature.
- Functional training: stair climbing, obstacle negotiation, sit-to-stand, and gait training on varied surfaces.
- Balance and agility drills.
- Aerobic/endurance training: walking, cycling, aquatic therapy, and possibly Tai Chi or Pilates for overall conditioning and balance.
- Self-guided home exercise programs with periodic supervision or telerehabilitation options.
- Patient education on lifestyle modification, pain management, and activity progression.
Exercises
- Advanced strengthening: leg press, lunges, step-ups, squats
- Balance: tandem walking, single leg stance on unstable surfaces, weight shifts
- Aerobic: treadmill walking, cycling, aquatic exercises
- Functional: stair climbing, sit-to-stand, walking on uneven surfaces
- Flexibility: hamstring, calf, hip flexor, and quadriceps stretches
- Mindfulness and stress reduction interventions as adjuncts if indicated.
Important Points
- Patient adherence to home exercise programs is crucial; telerehabilitation can be as effective as in-person therapy.
- Quality of life and satisfaction with care improve with appropriate rehabilitation but are comparable across various programs.
- Cognitive-behavioral approaches may help reduce kinesiophobia and improve outcomes.
- Progression of exercises should be based on patient-specific parameters assessed by clinicians.
Stage 4: Long-Term Maintenance Phase (After Month 3)
Goals
- Maintain strength, flexibility, and endurance
- Prevent falls and maintain balance
- Support return to higher-level activities and sports as appropriate
- Encourage lifelong physical activity to maintain joint health and overall wellness
Precautions
- Avoid overloading joint structures
- Monitor for signs of chronic pain or dysfunction
- Adjust exercise programs for comorbidities and aging
Interventions
- Continued strength and flexibility exercises
- Balance and proprioception exercises
- Cardiovascular conditioning
- Patient education on joint protection and activity modification
Exercises
- Resistance training (weights, elastic bands)
- Balance exercises (balance boards, dynamic stability tasks)
- Aerobic activities (walking, swimming, cycling)
- Functional exercises tailored to patient goals
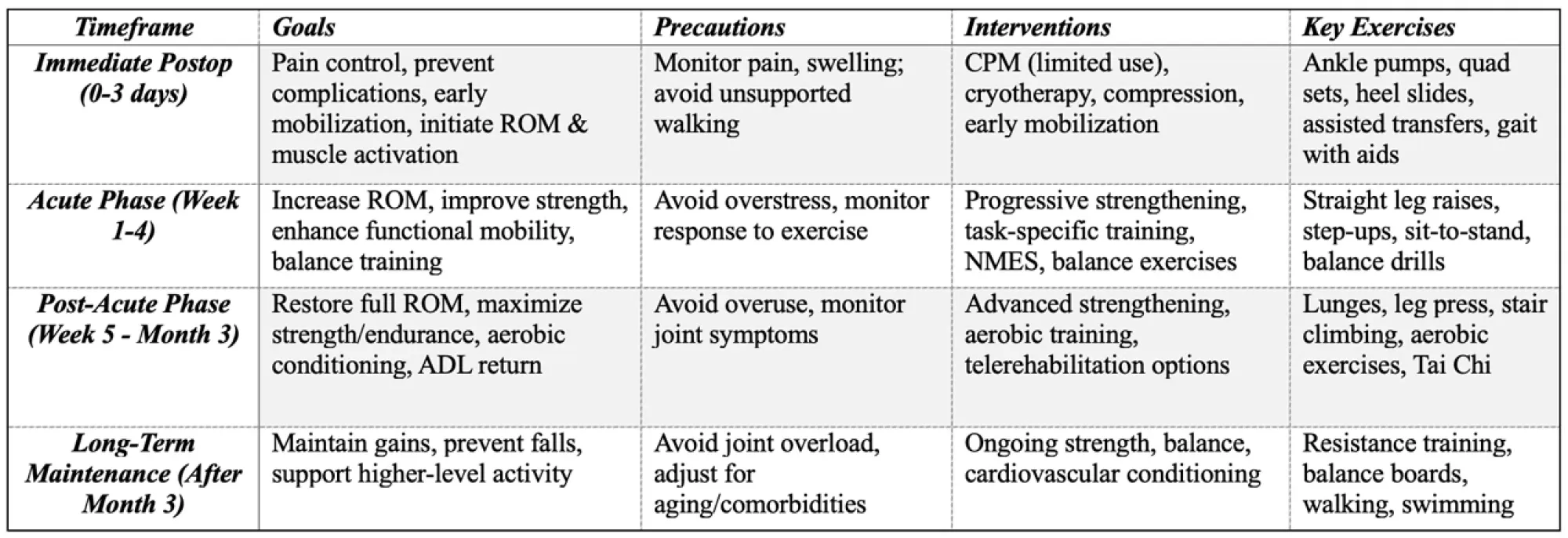
Summary Table of TKR Rehabilitation Protocol by Timeline
Additional Noteworthy Points
- Preoperative rehabilitation has been shown to significantly improve surgical outcomes.
- Preoperative exercise and education improve postoperative outcomes and reduce hospital stay.
- High-intensity and high-velocity exercises are safe and may lead to faster functional recovery.
- Telerehabilitation is an effective alternative to in-person therapy and can reduce costs.
- Early initiation of rehabilitation within 24 hours is associated with shorter length of stay and improved outcomes.
- Adjunctive therapies such as NMES and biofeedback can assist in muscle activation deficits.
- Balance training is important for reducing fall risk and improving gait.
- Rehabilitation protocols and outcomes remain heterogeneous; standardized reporting and core outcome sets are needed.
Reference:
- Konnyu, K. J., Thoma, L. M., Cao, W., Aaron, R. K., Panagiotou, O. A., Bhuma, M. R., Adam, G. P., Balk, E. M., & Pinto, D. (2023). Rehabilitation for total knee arthroplasty: A systematic review. American Journal of Physical Medicine & Rehabilitation, 102(1), 19–33. https://doi.org/10.1097/PHM.0000000000002008
- Dávila Castrodad, I. M., Recai, T. M., Abraham, M. M., Etcheson, J. I., Mohamed, N. S., Edalatpour, A., & Delanois, R. E. (2019). Rehabilitation protocols following total knee arthroplasty: A review of study designs and outcome measures. Annals of Translational Medicine, 7(Suppl 7), S255. https://doi.org/10.21037/atm.2019.08.15
- Lisi, C., Caspani, P., Bruggi, M., Carlisi, E., Scolè, D., Benazzo, F., & Dalla Toffola, E. (2015). Early rehabilitation after elective total knee arthroplasty. Acta Biomedica, 88(Suppl 4), 56–61. https://doi.org/10.23750/abm.v88i4-S.5154
- Jette, D. U., Hunter, S. J., Burkett, L., Langham, B., Logerstedt, D. S., Piuzzi, N. S., Poirier, N. M., Radach, L. J. L., Ritter, J. E., Scalzitti, D. A., Stevens-Lapsley, J. E., Tompkins, J., & Zeni Jr., J. (2020). Physical therapist management of total knee arthroplasty. Physical Therapy, 100(9), 1603–1631. https://doi.org/10.1093/ptj/pzaa099
- Murphy, J., Pritchard, M. G., Cheng, L. Y., Janarthanan, R., & Leal, J. (2018). Cost-effectiveness of enhanced recovery in hip and knee replacement: A systematic review protocol. BMJ Open, 8(3), e019740. https://doi.org/10.1136/bmjopen-2017-019740
- Morrell, A. T., Layon, D. R., Scott, M. J., Kates, S. L., Golladay, G. J., & Patel, N. K. (2021). Enhanced recovery after primary total hip and knee arthroplasty: A systematic review. The Journal of Bone and Joint Surgery. American Volume, 103(20), 1938–1947. https://doi.org/10.2106/JBJS.20.02169