Achilles tendon rupture rehabilitation aims to restore tendon healing, muscle strength, ankle range of motion (ROM), and ultimately safe return to sport (RTS). Recent evidence supports early weightbearing (WB) and early ankle mobilization to improve functional outcomes without increasing rerupture risk tendon elongation occurs predominantly within the first 6 months postoperatively, but early loading protocols do not significantly increase. Progressive strengthening and neuromuscular control are essential components for long-term recovery.
This detailed protocol integrates current evidence from randomized controlled trials, consensus statements, and systematic reviews to guide clinicians and physiotherapists through the phases of rehabilitation after Achilles tendon repair.
Not sure if surgery is the best option for an Achilles tendon rupture? Read our full article about Operative vs Non-operative Management of Acute Achilles Tendon Rupture.
Protection Phase
Movement Restoration
Strength Development
Return to Activity
Rehabilitation Stages
Phase 1: Immediate Postoperative Phase (0–2 Weeks)
Goals:
- Protect the surgical repair and wound healing
- Manage pain and swelling
- Prevent complications (e.g., deep vein thrombosis)
- Maintain proximal muscle activity and cardiovascular fitness
Interventions:
- Immobilize ankle in plantarflexion using a short leg splint, cast or CAM boot with 3 heel wedges (~6 cm total) to maintain equinus position.
- Non-weightbearing (NWB) or partial weightbearing (PWB) as per surgeon’s advice; most protocols allow no WB during this phase.
- Patient education on wound care and signs of infection
- Initiate isometric exercises for hip, knee, and core muscles
- Submaximal plantarflexion isometric contractions in boot or cast at end range plantarflexion to stimulate calf muscle activation without stressing repair.
- Use cryotherapy and elevation to manage swelling and pain
- Blood flow restriction training (BFRT) can be initiated on ipsilateral or contralateral limb to preserve muscle mass.
Boot Wearing Schedule:
- CAM boot with 3 heel wedges continuously (day and night)
In-Home Tips for Patients:
- Keep the limb elevated as much as possible to reduce swelling
- Avoid active dorsiflexion or stretching beyond neutral
- Practice gentle toe curls and isometric calf contractions in boot
- Maintain cardiovascular fitness with upper body exercises
- Monitor wound for redness, discharge, or increased pain
Exercise Examples for Physiotherapists:
- Hip abduction/adduction isometrics
- Quadriceps sets and straight leg raises
- Seated plantarflexion isometrics with boot on (biofeedback encouraged)
- Breathing and core stabilization exercises
- Initiate BFRT with low-load exercises (e.g., straight leg raises)
Milestones / Precautions:
– No active or passive dorsiflexion past neutral
– Monitor for infection, DVT
– Maintain ankle & foot hygiene
Phase 2: Controlled Mobilization Phase (2–6 Weeks)
Goals:
- Gradual Progress to full weightbearing (FWB) safely
- Initiate controlled ankle range of motion (ROM) avoiding dorsiflexion beyond neutral
- Continue pain and swelling management
- Maintain proximal and global strength
Interventions:
- Transition from NWB to tolerable FWB in CAM boot with heel wedges; WBAT typically allowed by 3 weeks, FWB by 6 weeks.
- Ankle active ROM exercises initiated, limiting dorsiflexion to neutral with knee flexed to 90° to avoid tendon elongation.
- Avoid passive dorsiflexion stretching until after 12 weeks.
- Begin gentle soft tissue mobilization around scars once healed
- Proximal strengthening and cardiovascular exercises continue
- Maintain heel wedges in boot; reduce 1 wedge per week starting at week 5 (total 3-4 weeks wearing wedges).
- Continue BFRT focusing on plantarflexors and proximal muscles.
Boot Wearing Schedule:
- CAM boot with gradually decreasing heel wedges: starting week 4, one wedge off every week (from 3 wedges to none by week 6)
In-Home Tips for Patients:
- Use crutches as needed to assist with WB progression
- Perform ankle pumps and gentle active ROM within limits
- Monitor for signs of elongation (feel tightness but no pain)
- Continue elevation and icing as needed
- Encourage compliance with weightbearing restrictions and exercise progression
Exercise Examples for Physiotherapists:
- Active ankle plantarflexion and dorsiflexion to neutral (knee flexed)
- Seated ankle isotonic exercises with elastic bands
- Double-leg heel raises in boot (partial weightbearing)
- Hip and core strengthening progressions
- Aquatic therapy or stationary cycling with boot on (~week 4–6)
- Submaximal isometric plantarflexion
- Neuromuscular electrical stimulation (NMES) for gastrocnemius activation
Milestones / Precautions:
– Avoid passive calf stretching
– Monitor resting ankle tension as proxy for tendon elongation
– Avoid premature full dorsiflexion
Phase 3: Early Rehabilitation Phase (6–12 Weeks)
Goals:
- Normalize gait mechanics
- Restore ankle dorsiflexion gradually without overstressing repair
- Improve calf muscle strength and endurance
- Progress proprioceptive training
Interventions:
- Transition to athletic shoe with heel lift (~1.5–3 cm)
- Gradual reduction of heel lift height under supervision
- Initiate double-leg heel raises progressing through full ROM.
- Begin single-leg heel raises around week 10–12 if tolerated.
- Proprioceptive exercises such as balance board, single-leg stance, and perturbation training.
- Continue aquatic therapy and use of anti-gravity treadmill if available.
- Avoid aggressive stretching beyond dorsiflexion neutral until after 12 weeks.
Boot Wearing Schedule:
- Discontinue boot around 8 weeks (as per orthopedic team recommendation), transition to sneaker with heel lift (~1.5–3 cm).
- Use sneaker with heel lift during gait training until full ROM and strength achieved.
In-Home Tips for Patients:
- Focus on quality of gait; avoid limping or compensatory patterns
- Perform balance exercises safely near support
- Continue controlled calf strengthening avoiding pain
- Use compression socks and elevate limb to reduce swelling
Exercise Examples for Physiotherapists:
- Double-leg heel raises, progressing to slow eccentric lowering
- Single-leg heel raises (supported initially)
- Balance exercises: single-leg stance on stable and unstable surfaces
- Seated and standing calf strengthening with increasing load
- Stationary bike without boot, elliptical
- Initiate low-impact cardiovascular training (swimming, walking, Elliptical, stair climbing, treadmill walking)
Submaximal Isometric Ankle PF in Shortened Position
Seated Ankle PF Isotonics
Leg Press Ankle PF
Double Leg Calf Raise
SL Supported Calf Raise
SL Calf Raise
SL Deficit Calf Raise
Sample Ankle Plantar Flexion Progression (Marrone et al., 2024)
Milestones / Precautions:
– Heel raise height and repetitions gradually increase
– Monitor for compensatory movement patterns
– Avoid excessive dorsiflexion stretching
Phase 4: Late Rehabilitation Phase (12–24 Weeks)
Goals:
- Restore full ankle ROM including dorsiflexion
- Achieve calf muscle strength >70–80% limb symmetry index (LSI)
- Initiate plyometric and running progression
- Improve neuromuscular control and endurance
Interventions:
- Remove heel lift when ankle dorsiflexion reaches near normal
- Progressive resistance exercises for calf with emphasis on eccentric loading.
- Plyometric training introduction with low amplitude activities (e.g., pogo jumps, ladder drills).
- Running progression starting typically at 12–16 weeks post-op based on strength and control.
- Continue proprioceptive and balance training with dynamic challenges
- Monitor tendon elongation via clinical signs and resting ankle position.
Boot Wearing Schedule:
- No boot; normal shoe wear with gradual reduction of heel lift as ROM improves.
In-Home Tips for Patients:
- Continue gradual loading and plyometric drills as instructed
- Avoid sudden increases in activity to prevent overloading
- Focus on movement quality to prevent compensatory patterns
- Use ice and compression after higher load days if needed
Exercise Examples for Physiotherapists:
- Single-leg heel raises progressing to multiple repetitions
- Plyometric drills: Ladder drills, band-assisted pogo jumps, box jumps, drop jumps (progressive), triple extension drills
- Running progression (typically from 12-16 weeks)
- Running drills: straight-line jogging, gradual increase in volume
- Functional strengthening: lunges, step-ups, mini-squats, Bulgarian split squats, hip strengthening
- Use force plates or biofeedback devices to assess and train symmetry
Milestones / Precautions:
– Achieve controlled gait mechanics
– Strength benchmarks before running: 1.5-2.0x body weight seated plantarflexion
– Use aquatic and anti-gravity treadmill as needed
Phase 5: Return to Sport Phase (24+ Weeks)
Goals:
- Achieve >90% strength and endurance compared to contralateral side
- Progress training volume and sport-specific skills
- Safely return to full sports participation
Interventions:
- Isokinetic and isometric strength testing to confirm readiness (>90% LSI recommended)
- Advanced plyometric and agility drills with reactive components
- Sport-specific training under supervision
- Monitoring workload and fatigue to prevent reinjury
Boot Wearing Schedule:
- None
In-Home Tips for Patients:
- Adhere strictly to progression guidelines
- Pay attention to pain or swelling after activity
- Maintain strength and flexibility programs
- Communicate concerns promptly with therapist or surgeon
Exercise Examples for Physiotherapists:
- High-level plyometrics: drop jumps, bounding
- Reactive agility drills and neurocognitive training (drop vertical jumps, RSI monitoring)
- Progressive running drills including changes in direction and speed
- Strength and conditioning focusing on power (e.g., loaded calf raises)
- Isokinetic/isometric strength testing
- On-field/court sport-specific drills and conditioning
- Functional testing: single-leg hop, heel-rise endurance tests
- Neurocognitive and reactive training to prepare for sport demands
Milestones / Precautions:
– Strength: >90% LSI and 1.5-2.0x BW plantarflexion force
– Heel-rise endurance >90% LSI
– Monitor for calf endurance deficits and tendon elongation
– Progressive chronic load management
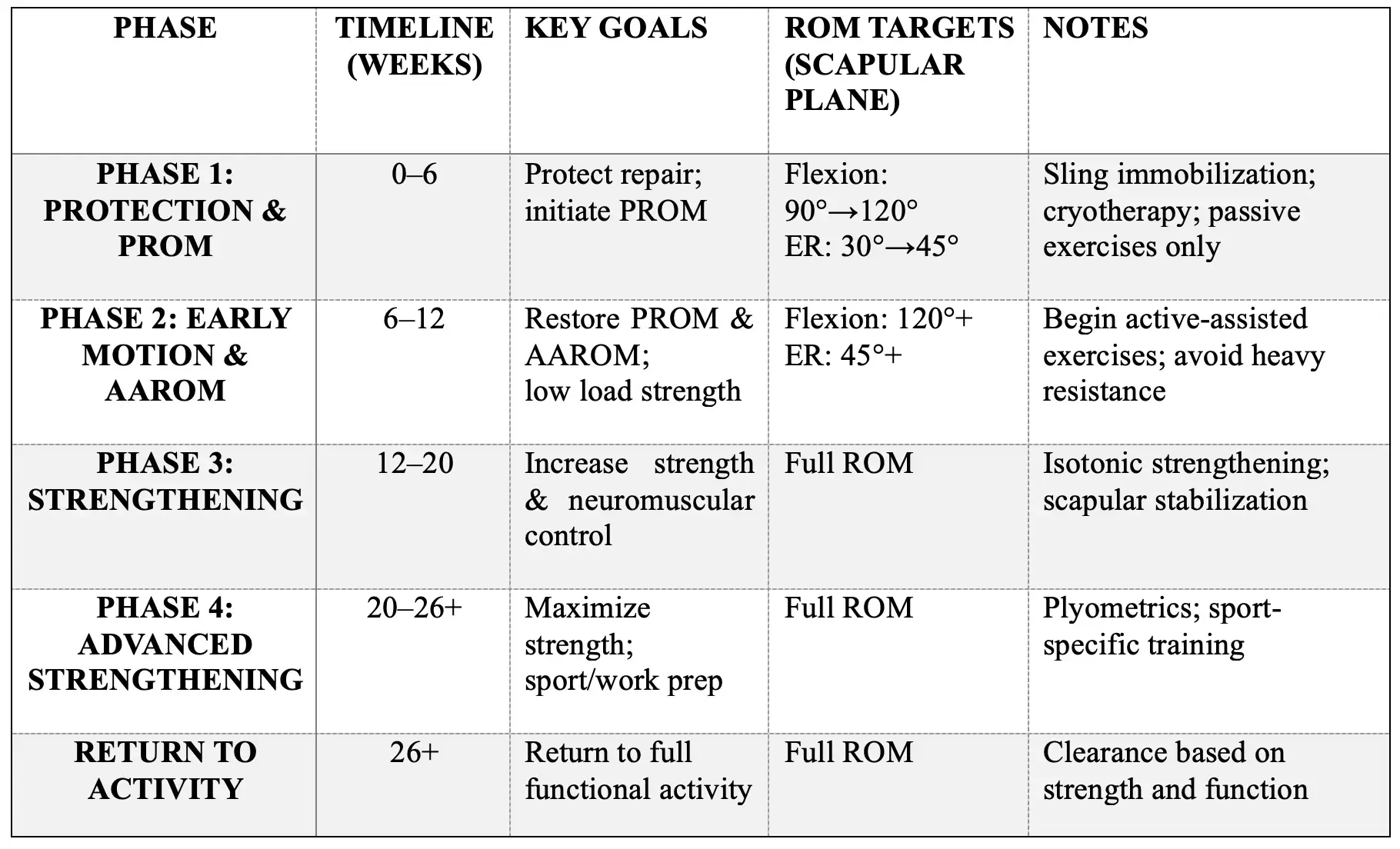
Summary Table of Exercises per Category and Timeline
New Findings and Considerations for Physiotherapists
- Early Weightbearing & Mobilization: Immediate or early weightbearing (within first 1–2 weeks) with controlled ankle motion is safe, does not increase re-rupture risk, and may accelerate functional recovery
- Tendon Elongation: Tendon elongation continues for up to 6 months postoperatively regardless of early or late weightbearing protocols and is a key factor influencing long-term function
- Blood Flow Restriction Training (BFRT): BFRT during early rehab can preserve muscle strength and promote hypertrophy with low loads, beneficial when high-load exercises are contraindicated
- Use of Biofeedback & Objective Measures: Devices such as force plates and isokinetic dynamometers provide valuable feedback for strength and symmetry and should be incorporated when possible
- Gradual Reduction of Heel Wedges: Heel wedges in boots and shoes help protect the repair by maintaining slight plantarflexion; a gradual reduction over 4–6 weeks is crucial to avoid elongation
- Avoid Excessive Dorsiflexion Stretching: Passive dorsiflexion stretching should be avoided until at least 12 weeks to prevent tendon elongation
- Long-Term Rehabilitation: Full recovery of muscle strength, endurance, and patient-reported function may take 12 months or longer
- Return to Sport (RTS) as a Continuum: RTS should be considered a progressive continuum with objective testing guiding decisions rather than time alone
Reference:
- Lee, K. W., Bae, J.-Y., Ho, B. C., Kim, J. H., & Seo, D.-K. (2022). Immediate weightbearing and ankle motion exercise after acute Achilles tendon repair. The Journal of Foot & Ankle Surgery, 61(5), 604–608. https://doi.org/10.1053/j.jfas.2021.10.021
- Saxena, A., Giai Via, A., Silbernagel, K. G., Walther, M., Anderson, R., Gerdesmeyer, L., & Maffulli, N. (2022). Current consensus for rehabilitation protocols of the surgically repaired acute mid-substance Achilles rupture: A systematic review and recommendations from the “GAIT” study group. The Journal of Foot & Ankle Surgery, 61(6), 855–861. https://doi.org/10.1016/j.jfas.2021.12.008
- Massen, F. K., Shoap, S., V., J. T., Fan, W., Usseglio, J., Baumbach, S. F., & Polzer, H. (2022). Rehabilitation following operative treatment of acute Achilles tendon ruptures: A systematic review and meta-analysis. EFORT Open Reviews, 7(10), 680–691. https://doi.org/10.1530/EOR-22-0072
- Kiedrowski, B., Bąkowski, P., Stołowski, Ł., Kaszyński, J., & Kerkhoff, G. (2021). Rehabilitation protocol after Achilles tendon reconstruction with an autologous hamstring graft. Issues of Rehabilitation, Orthopaedics, Neurophysiology and Sport Promotion, 37, 43–50. https://doi.org/10.19271/IRONS-000146-2021
- Gould, H. P., Bano, J. M., Akman, J. L., & Fillar, A. L. (2021). Postoperative rehabilitation following Achilles tendon repair: A systematic review. Sports Health, 29(3), 130–145. https://doi.org/10.1097/JSA.000000000000030
- Marrone, W., Andrews, R., Reynolds, A., Vignona, P., Patel, S., & O’Malley, M. (2024). Rehabilitation and return to sports after Achilles tendon repair. International Journal of Sports Physical Therapy, 19(9), 1152–1171. https://doi.org/10.26603/001c.122643
- Eliasson, P., Agergaard, A. S., Couppé, C., Svensson, R., Hoe, H., Warming, S., … & Magnusson, S. P. (2018). The ruptured Achilles tendon elongates for six months after surgical repair regardless of early or late weightbearing in combination with ankle mobilization: A randomized clinical trial. The American Journal of Sports Medicine, 46(10), 2492–2502. https://doi.org/10.1177/0363546518776588

