Unlocking Recovery: The Role of Neuroplasticity After ACL Reconstruction and How to Harness It for Better Outcomes
What is Neuroplasticity?
Why is Neuroplasticity Important After ACL Reconstruction?
After an ACL injury and surgery, patients often experience a reduction in somatosensory feedback—information from receptors in the knee about joint position and movement. To compensate, the brain increases reliance on visual feedback (using the eyes) to guide knee movements. While this compensatory strategy helps maintain function initially, it can overload the brain’s motor control systems, especially during fast, complex sports movements, increasing the risk of reinjury.
Traditional rehabilitation programs primarily focus on restoring muscle strength and joint mechanics but may overlook these important changes in brain function and sensory integration. Without addressing neuroplastic adaptations, patients may unknowingly continue to rely heavily on vision for movement control, which can limit their recovery and increase vulnerability to subsequent injury.
Visual Explanation: Traditional vs. Integrated Training Approaches
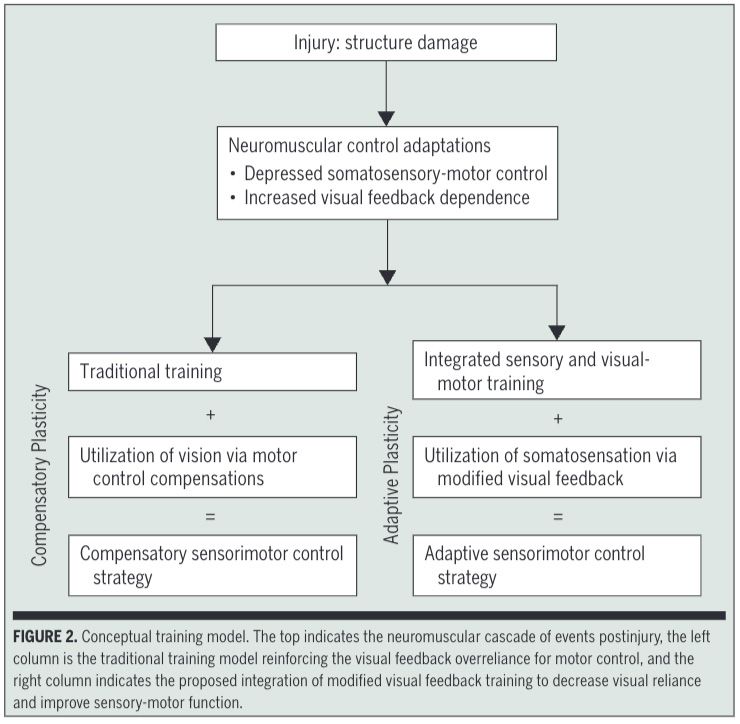
Figure 1: Traditional training (left) reinforces overreliance on vision for motor control, leading to compensatory sensorimotor strategies. Integrated sensory and visual-motor training (right) modifies visual feedback to encourage the brain to use somatosensory inputs, promoting adaptive neuroplasticity and improved functional outcomes.
- Traditional Training: Focuses on neuromuscular exercises but continues to rely heavily on vision. This leads to compensatory plasticity, where the brain reinforces the dependence on visual cues.
- Integrated Sensory and Visual-Motor Training: Combines sensory retraining with modified visual feedback to promote the use of somatosensory information. This encourages adaptive plasticity, improving sensorimotor control and function.
Neural Compensation and Cognitive-Motor Challenges
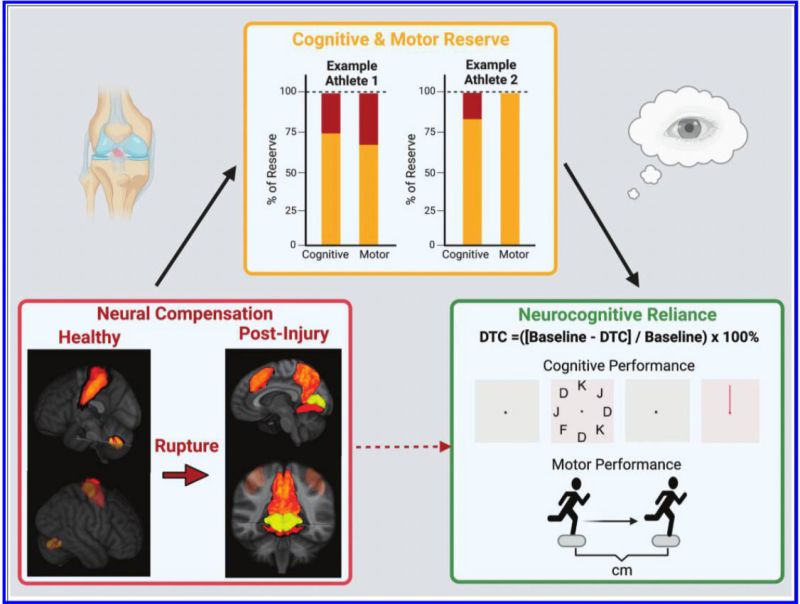
Figure 2: Athletes with lower cognitive and motor reserves show increased neural compensation and neurocognitive reliance post-ACL injury, as evidenced by higher dual-task cost (performance decline when cognitive tasks are added to motor tasks).
- Athletes with less cognitive and motor reserve may rely more on neurocognitive resources to maintain movement control.
- This increased reliance is measurable using dual-task testing, where motor performance declines when a cognitive task is added, indicating the brain’s compensatory efforts.
- Understanding these dynamics is crucial for assessing readiness to return to sport, as it highlights the need for integrating cognitive and motor recovery.
Strategies to Harness Neuroplasticity and Optimize Rehab
To address the neuroplastic changes after ACL reconstruction and improve recovery, early interventions should include:
- Neurocognitive Training: Incorporate exercises that challenge attention, memory, and decision-making during physical tasks to enhance cognitive-motor integration.
- Proprioceptive and Balance Exercises: Use balance boards, single-leg stances, and dynamic stability drills to retrain joint position sense and neuromuscular control.
- Visual-Motor Coordination: Engage in activities requiring visual tracking and coordination, such as catching or reacting to moving objects, to strengthen sensorimotor pathways.
- External Focus of Attention: Encourage patients to focus on the effects of their movements (e.g., landing softly) rather than the movements themselves, promoting automaticity and efficient motor patterns.
- Dual-Task Training: Combine physical exercises with cognitive challenges (e.g., counting backward while balancing) to simulate real-world sport demands and improve functional performance.
Integrating these strategies alongside traditional strength and functional training can reduce overreliance on vision, improve sensory integration, and help patients regain more natural motor control, ultimately reducing reinjury risk.
Conclusion
References
- Wilk, K. E., Ivey, M., Thomas, Z. M., & Lupowitz, L. (2024). Neurocognitive and Neuromuscular Rehabilitation Techniques after ACL Injury, Part 1: Optimizing Recovery in the Acute Post-Operative Phase-A Clinical Commentary. International Journal of Sports Physical Therapy, 19(11), 1373.
- Grooms, D., Appelbaum, G., & Onate, J. (2015). Neuroplasticity following anterior cruciate ligament injury: A framework for visual-motor training approaches in rehabilitation. Journal of Orthopaedic & Sports Physical Therapy, 45(5), 381–393.
- Grooms, D. R., Chaput, M., Simon, J. E., Criss, C. R., Myer, G. D., & Diekfuss, J. A. (2023). Combining neurocognitive and functional tests to improve return-to-sport decisions following ACL reconstruction. Journal of Orthopaedic & Sports Physical Therapy, 53(8), 415–419.