Proximal humerus fractures (PHFs), injuries involving the upper portion of the arm bone near the shoulder, are a common clinical condition, especially among older adults. This article provides a clear and structured overview of PHFs, including epidemiology, risk factors, diagnostic methods, classification, treatment options, rehabilitation principles, and potential complications. All information is derived from high-quality academic sources to support students, clinicians, and individuals seeking to better understand these injuries.
What Are Proximal Humerus Fractures?
Epidemiology and Risk Factors
PHFs account for approximately 5–6% of all adult fractures, making them the third most common fracture type in older adults after hip and distal radius fractures. Their incidence continues to rise globally due to population aging.
- Age and Gender: Older adults—particularly women—are at greater risk due to osteoporosis and increased fall risk. Incidence reaches up to 711.8 per 100,000 person-years in women over age 85.
- Mechanism of Injury: PHFs show a bimodal distribution:
-
- Younger adults: High-energy trauma
- Older adults: Low-energy falls
Associated Risks: Patients with a PHF have an elevated risk for subsequent fractures (e.g., hip fractures), often due to impaired neuromuscular control and underlying bone health issues.
How Are Proximal Humerus Fractures Diagnosed?
Clinical Evaluation
A thorough patient history is essential, emphasizing mechanism of injury, functional demands, and comorbidities. Neurovascular assessment is critical due to the proximity of the axillary nerve.
Imaging
- X-rays: Standard Views include AP (Grashey), scapular Y, and axillary views.
- CT Scans: Useful for complex or comminuted fractures to better define patterns.
- MRI: Typically reserved for soft tissue evaluation rather than acute fracture assessment.
Treatment Options for Proximal Humerus Fractures
Management depends on patient age, health status, functional goals, fracture displacement, and surgeon preference.
1. Nonoperative Management
Indications: Minimally displaced or stable fractures, and patients who are poor surgical candidates.
Approach:
- Sling immobilization
- Early, progressive physical therapy (Hodgson, 2006)
Outcomes:
Most patients achieve satisfactory recovery. However, some may experience reduced shoulder function compared with operative cases, depending on fracture type.
Potential Complications:
- Stiffness
- Nonunion or malunion
- Rotator cuff dysfunction
- Impaired motion from prolonged immobilization
2. Operative Management
The following surgical methods are most performed to manage proximal humerus fractures:
- Closed Reduction and Percutaneous Pinning (CRPP)
- Open Reduction and Internal Fixation (ORIF)
- Intramedullary Nailing (IMN)
- Shoulder Arthroplasty:
-
- Hemiarthroplasty (HA)
- Reverse Total Shoulder Arthroplasty (RSA)
Indications
Operative management is generally considered for displaced, unstable, comminuted fractures; fracture-dislocations; head-split fractures; cases with vascular compromise; or when nonoperative management is not expected to restore adequate function.
Outcomes
Studies show mixed results. Some displaced or complex fracture patterns may benefit functionally from surgery, although outcomes vary depending on fracture severity, bone quality, and patient-related factors.
Complications of Operative Management
- After ORIF: mechanical failure, screw cut-out, avascular necrosis, infection, nonunion, malunion, postoperative stiffness.
- After RSA: dislocation, scapular notching, infection, loosening of components, tuberosity nonunion.
Careful patient selection, appropriate surgical technique, and postoperative rehabilitation are essential in minimizing these complications.
Age-Related Outcomes in Conservative Management
Age-related outcomes are an important consideration in determining appropriate management for proximal humerus fractures. Evidence consistently shows that older age is associated with less favorable outcomes following conservative (non-operative) treatment, largely due to poor bone quality, reduced healing capacity, and higher fracture complexity in elderly patients. Several studies demonstrate that patients over 65 have higher rates of functional limitations, persistent pain, and complications such as malunion or delayed healing when managed non-operatively compared to younger patients with similar fracture patterns. These findings highlight the importance of individualized treatment planning, as older adults may benefit from earlier consideration of operative options, while still recognizing that many elderly patients continue to achieve satisfactory outcomes without surgery when fracture stability and displacement criteria are met.
How Has PHF Management Evolved Over Time?
Large population-based research demonstrates that:
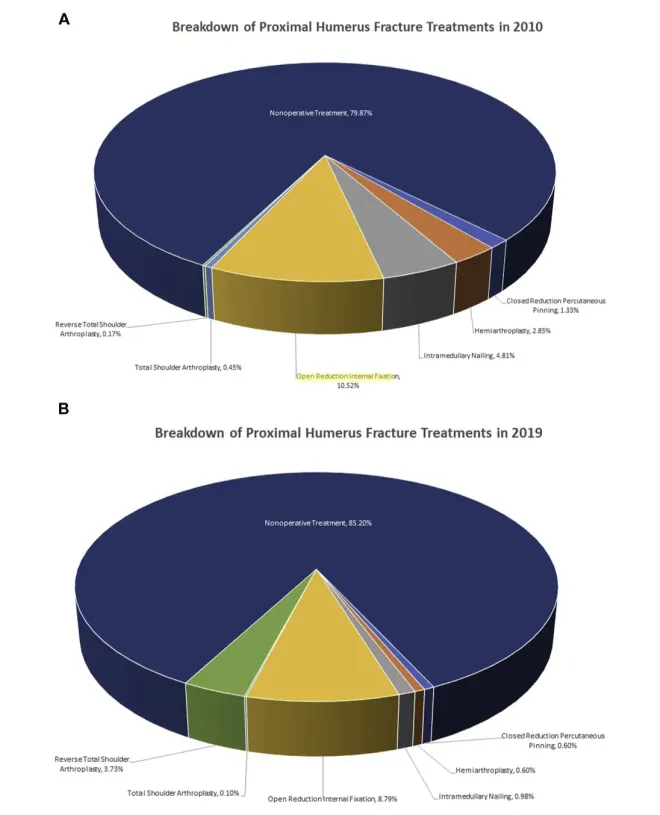
- More than 80% of elderly PHF cases continue to be managed nonoperatively.
- Between 2010 and 2019, nonoperative rates increased further.
- RSA use in older adults has risen dramatically, an increase of over 1800% over the decade.
- Use of other operative methods has declined.
Role of Rehabilitation in PHF Management
Early rehabilitation is essential to prevent stiffness and optimize functional recovery. Strong evidence suggests that immobilization beyond 1–2 weeks offers no additional benefit.
Rehabilitation Phases
Early Phase (0–2 weeks):
- Education
- Pain management
- Gravity-assisted pendulum exercises
Intermediate Phase (2–8 weeks):
- Passive ROM exercises
- Proprioceptive training
Late Phase (>8 weeks):
- Active ROM
- Strengthening
- Functional tasks
Home exercise programs are effective, especially for older adults with limited access to physiotherapy.
You can check out our articles to learn more about the rehabilitation protocol for this fracture, non-operative management and post-operative management.
Most Common Complications After PHFs
After ORIF:
- Mechanical failure
- Avascular necrosis
- Infection
- Nonunion or malunion
- Stiffness
After RSA:
- Dislocation
- Scapular notching
- Infection
- Component loosening
- Tuberosity nonunion
Appropriate surgical technique and postoperative protocols can mitigate many of these risks.
Clinical Implications
Proximal humerus fractures are increasingly common, especially in older adults, with incidence rising due to aging populations. Management must be individualized based on fracture characteristics, bone quality, comorbidities, functional demand, and patient preference.
The literature emphasizes several key clinical considerations:
- Nonoperative management remains the first-line treatment for most proximal humerus fractures (approximately 65–85%), especially stable, minimally displaced fractures or patients with significant medical comorbidities.
- Patients may choose or be advised nonoperative treatment first and then undergo delayed surgery if complications arise (e.g., nonunion, malunion, persistent pain, failure to regain function).
- Early surgery (ideally within the first month) is recommended when operative intervention is clearly indicated (fracture-dislocations, head-split fractures, vascular injury, or significant displacement). This timeframe represents the acute management window identified in large database studies.
- Rehabilitation is essential, regardless of treatment choice. Evidence supports:
-
- early mobilization (within 1–2 weeks),
- progressive loading,
- proprioceptive retraining,
- and patient education to prevent prolonged stiffness and functional decline.
- Osteoporosis and fall-risk management should be integral to long-term care, as PHFs often signal underlying fragility and increased risk of subsequent fractures (hip, wrist, spine).
- Shared decision-making is critical. Treatment decisions should reflect:
-
- patient goals,
- functional demands,
- fracture severity,
- medical status,
- lifestyle,
- and anticipated rehabilitation potential.
In summary, proximal humerus fracture management is highly individualized. Nonoperative treatment is appropriate for most patients, with surgery reserved for specific indications or cases where conservative treatment fails. Rehabilitation plays a central role in maximizing recovery and function.
Reference:
- Baker, H. P., Gutbrod, J., Strelzow, J. A., Maassen, N. H., & Shi, L. (2022). Management of proximal humerus fractures in adults-a scoping review. Journal of Clinical Medicine, 11(20), 6140. https://doi.org/10.3390/jcm11206140
- Barlow, J. D. (2021). Complications after ORIF of proximal humerus fractures-how to deal with them. Annals of Joint, 6, 16. https://doi.org/10.21037/aoj-20-77
- Budharaju, A., Hones, K. M., Hao, K. A., Wright, J. O., Fedorka, C. J., Kaar, S. G., Bohsali, K. I., Wright, T. W., Patrick, M. R., & King, J. J. (2024). Rehabilitation protocols in proximal humerus fracture management: A systematic review. Shoulder & Elbow, 16(4), 449-458. https://doi.org/10.1177/17585732231182374
- Ferrel, J. R., Trinh, T. Q., & Fischer, R. A. (2015). Proximal humerus fractures in the elderly: Conservative versus operative treatment. Journal of Shoulder and Elbow Surgery, 24(10), 1728–1736. https://doi.org/10.1016/j.jse.2015.04.018
- Hodgson, S. A. (2006). Proximal humerus fracture rehabilitation. Clinical Orthopaedics and Related Research, 442, 131-138. https://doi.org/10.1097/01.blo.0000194677.02506.45
- Patel, A. H., Wilder, J. H., Ofa, S. A., Lee, O. C., Savoie, F. H., O’Brien, M. J., & Sherman, W. F. (2022). Trending a decade of proximal humerus fracture management in older adults. JSES International, 6(2), 137-143. https://doi.org/10.1016/j.jseint.2021.08.006