Proximal humerus fractures (PHFs) are among the most common fragility fractures in adults, particularly prevalent in the elderly population, with incidence increasing over recent decades due to aging demographics. Non-operative management remains the mainstay treatment for the majority of these fractures, surpassing operative interventions in frequency, especially in patients with minimally displaced or stable fractures. Despite advances in surgical techniques, evidence from randomized controlled trials and meta-analyses consistently shows no clear superiority of surgery over conservative treatment in elderly patients, with non-operative treatment associated with fewer complications and revision surgeries. Rehabilitation, therefore, becomes a critical component to optimize functional recovery, minimize pain, and restore independence in activities of daily living (ADLs). To study more about the differences between these operative and non-operative management of PHFs, read our other article, Understanding Proximal Humerus Fractures.
This protocol provides a comprehensive, evidence-based, phased approach aimed at physiotherapists and patients to guide rehabilitation following non-operative management of PHFs.
Rehabilitation Protocol
Phase 1: Acute Phase (Week 1)
Goal:
- Provide immobilization for pain relief and fracture stability.
- Minimize swelling and prevent stiffness in adjacent joints.
- Educate patient on injury and rehabilitation expectations.
Interventions:
- Immobilize the shoulder using an arm sling or a Gilchrist bandage, ensuring comfort and avoiding excessive tightness to prevent neurovascular compromise.
- Encourage active movement of fingers, wrist, and elbow to maintain mobility and circulation.
- Patient education on safe movements, pain management, and positioning (e.g., semi-reclined position for sleeping).
- Use of an axillary roll or pillow to counteract medial displacement forces from the pectoralis major muscle may be considered.
Immobilization:
- Arm sling or Gilchrist bandage; consider plaster reinforcement for unstable fractures.
- Immobilization in slight external rotation may reduce tuberosity displacement.
- Depending on the type of fracture and degree of deformity, different forms of immobilization may be required for the patient’s arm. Please refer to the examples below.
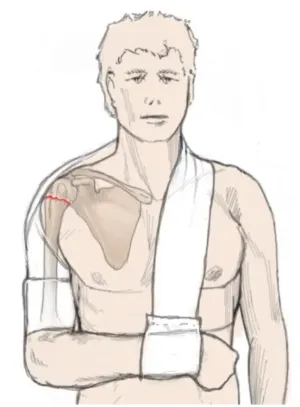
Simple Fracture: Patient with an arm sling. In this commercially available version, the upper arm and forearm are free and not encircled by the bandage as would be the case with the classic Gilchrist bandage (Razaeian et al., 2022)
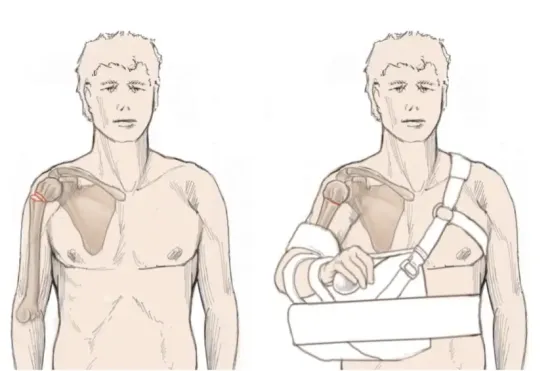
Varus-displaced fractures and/or greater tuberosity involvement: Patient with varus dis-placed fracture before (left) and after (right) application of the abduction orthosis. In this example, the humeral shaft is adjusted to the displaced humeral head fragment by abduction of the arm (Razaeian et al., 2022)
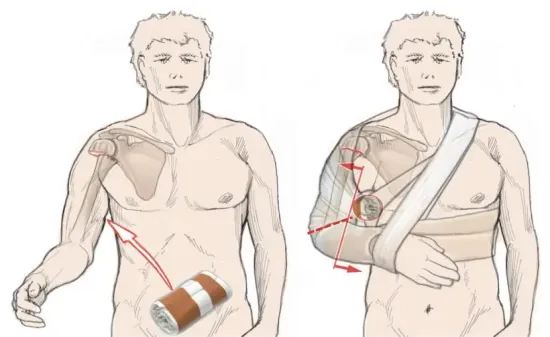
Counteract medial displacement: Patient with medial shaft translation before (left) and after (right) application of a Gilchrist bandage and axillary roll (Razaeian et al., 2022)
Precautions:
- Avoid active shoulder movements that could compromise fracture stability.
- Monitor for signs of neurovascular compromise or excessive swelling.
- Immobilization should not exceed 3-4 weeks to reduce risk of stiffness.
Exercise Examples:
- Active finger flexion and extension.
- Wrist circles and flexion/extension.
- Elbow flexion and extension within pain tolerance.
- Gentle grip strengthening using a soft ball or putty to maintain hand function.
Phase 2: Early Mobilization Phase (Weeks 2–3)
Goal:
- Initiate pain-controlled passive shoulder mobilization.
- Maintain mobility of adjacent joints.
- Promote fracture healing through gentle movement.
Interventions:
- Transition to a more comfortable support such as a shoulder bag/slings with less restrictive immobilization.
- Begin Codman pendulum exercises to facilitate passive shoulder movement without stressing fracture fragments.
- Initiate therapist-assisted or contralateral arm-assisted passive range of motion (PROM) exercises focusing on forward elevation and abduction to approximately 30–60 degrees within pain limits.
- Continue active movements of elbow, wrist, and fingers.
- Encourage postural training and scapular retraction exercises.
Immobilization:
- Use of shoulder bag or sling for comfort; removed during exercise and hygiene.
- Immobilization duration generally reduced to approximately 1–2 weeks.
Precautions:
- Avoid active shoulder abduction or rotation beyond pain-free limits.
- Monitor for pain increase or signs of fracture displacement.
- No strengthening exercises at this stage.
Exercise Examples:
- Codman pendulum exercises: side-to-side, circular, and front-to-back motions.
- Passive forward elevation in supine (“prayer position”), starting at 30 degrees and progressing as tolerated.
- Passive external rotation to 20 degrees, avoiding pain.
- Scapular setting: gentle scapular retraction and depression.
Phase 3: Active Mobilization Phase (Weeks 4–6)
Goal:
- Restore active range of motion (AROM) of the shoulder.
- Begin functional use of the arm in ADLs.
- Reduce pain and improve joint nutrition.
Interventions:
- Discontinue immobilization aids as tolerated; encourage use of arm in daily activities.
- Progress to active-assisted range of motion (AAROM) exercises transitioning to active range of motion.
- Initiate gentle isometric strengthening of the rotator cuff and scapular stabilizers (deltoid, supraspinatus, infraspinatus, teres minor, subscapularis) within pain limits.
- Continue PROM exercises as needed for any restricted planes.
- Encourage functional tasks such as reaching at waist and chest level.
Immobilization:
- Sling use discontinued or used only for comfort during prolonged inactivity.
Precautions:
- Avoid heavy lifting or resisted exercises beyond patient’s tolerance.
- Monitor for any increased pain or signs of malunion or nonunion.
- Avoid combined overhead activities if pain or instability present.
Exercise Examples:
- Active forward elevation up to 90°.
- Active abduction up to 90°.
- Active external and internal rotation within pain-free range.
- Isometric shoulder flexion, extension, abduction, and rotation exercises (hold contractions for 5–10 seconds).
- Scapular retraction exercises with resistance bands (light).
- Wall slides and finger ladder exercises for shoulder mobility.
Phase 4: Strengthening and Functional Integration Phase (Weeks 7–12)
Goal:
- Achieve near-normal shoulder range of motion.
- Improve shoulder strength and endurance.
- Restore functional use for ADLs and occupational tasks.
Interventions:
- Begin progressive resistive strengthening exercises focusing on rotator cuff and scapular muscles.
- Incorporate proprioceptive and neuromuscular control exercises.
- Introduce overhead and weight-bearing activities as tolerated.
- Encourage use of shoulder pulley systems, stretching, and scapulothoracic mobilization.
- Begin supervised physiotherapy sessions if available; continue home-based exercises.
Immobilization:
- No immobilization.
Precautions:
- Avoid painful activities; progress intensity gradually.
- Monitor for signs of impingement or overuse injuries.
- Avoid heavy lifting (>2-3 kg) until adequate strength and control achieved.
Exercise Examples:
- Theraband or light dumbbell external and internal rotation strengthening.
- Shoulder flexion and abduction with resistance bands or light weights.
- Scapular stabilization exercises: rows, scapular punches.
- Closed chain exercises: wall push-ups, weight shifting.
- Shoulder pulley exercises for elevation and rotation.
- Stretching exercises for posterior capsule and pectoralis minor to prevent tightness.
Additional Recommendations and Considerations
- Early Mobilization: Recent evidence supports early mobilization (within 1 week) to improve short-term outcomes without increasing complications.
- Pain Management: Pain is a significant barrier to compliance; optimizing analgesia including potential use of regional blocks (e.g., interscalene block) may enhance participation.
- Patient Education: Educate patients on the expected course, importance of compliance, and realistic functional goals to improve motivation and adherence.
- Monitoring and Follow-up: Regular clinical and radiographic follow-up at approximately 1, 3, 6, and 12 weeks is recommended to detect secondary displacement or complications.
- Rehabilitation Compliance: Compliance strongly predicts better clinical outcomes, especially in the short term. Strategies to improve adherence include pain control, social support, and simplified exercise regimens.
- Adaptation for Elderly: Protocols should be individualized considering cognitive status, comorbidities, and social support to ensure safety and optimize outcomes.
- Avoid Prolonged Immobilization: Extended immobilization (>4 weeks) increases risk of stiffness and functional limitation.
Summary Table: Rehabilitation Protocol for Non-Operative Management of Proximal Humerus Fractures
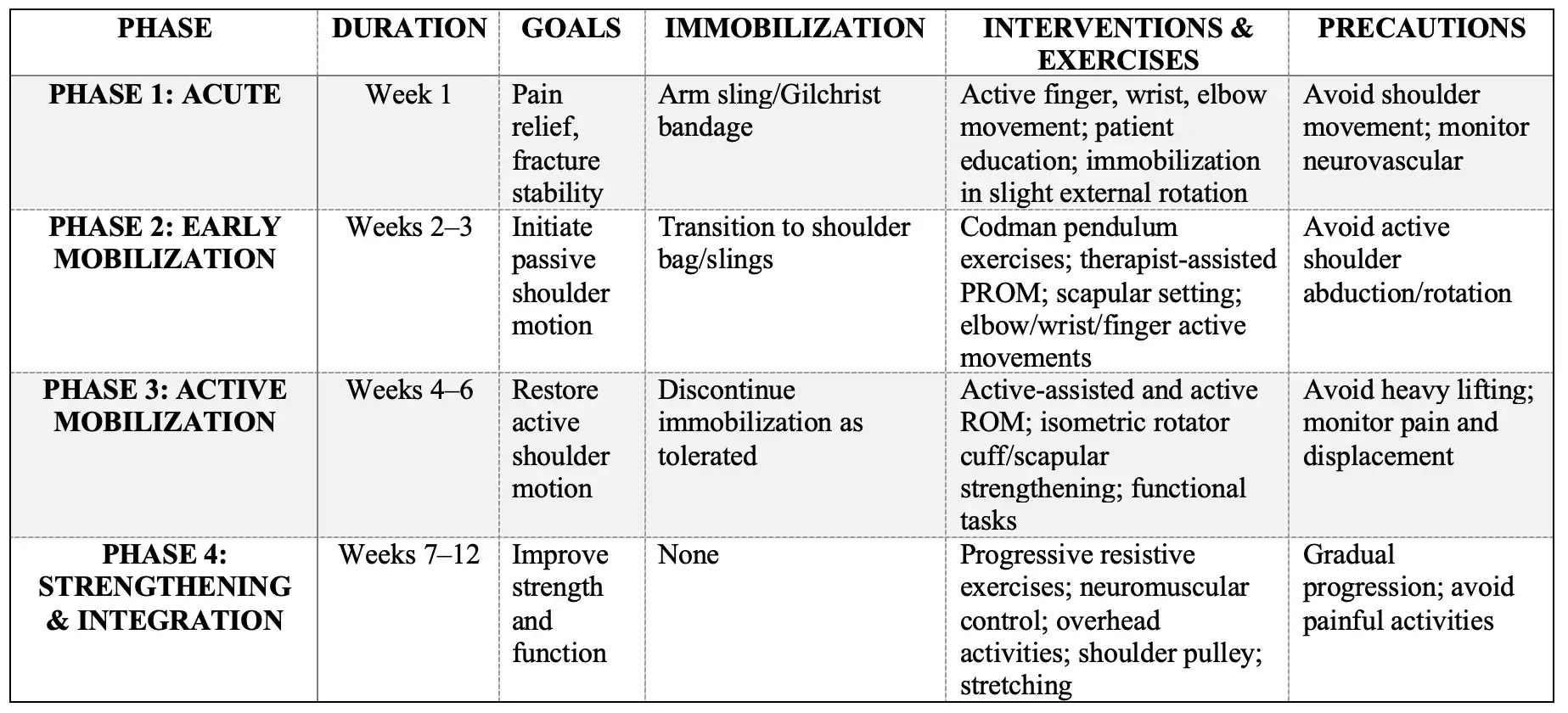
Conclusion
Reference:
- Aguado, H. J., Ariño, B., Moreno-Mateo, F., Bustinza, E. Y., Simón-Pérez, C., Martínez-Zarzuela, M., et al. (2018). Does an early mobilization and immediate home-based self-therapy exercise program displace proximal humeral fractures in conservative treatment? Observational study. Journal of Shoulder and Elbow Surgery, 27(11), 2021-2029. https://doi.org/10.1016/j.jse.2018.04.001
- Brorson, S. (2021). Evidence-based orthopedics and the myth of restoring the anatomy. Acta Orthopaedica, 92(5), 505-506. https://doi.org/10.1080/17453674.2021.1966916
- Martínez, R., Santana, F., Pardo, A., & Torrens, C. (2021). One versus 3-week immobilization period for nonoperatively treated proximal humeral fractures: a prospective randomized trial. Journal of Bone and Joint Surgery American, 103(16),1491-1498. https://doi.org/10.2106/JBJS.20.02137
- Martinez-Catalan, N. (2023). Conservative treatment of proximal humerus fractures: When, how, and what to expect. Current Reviews in Musculoskeletal Medicine, 16(1), 75-84. https://doi.org/10.1007/s12178-022-09817-9
- Nah, M. F. K., Pereira, M. J., Hemaavathi, M., Wong, S. W., Lim, C. J., & Tan, B. Y. (2023). Study on proximal humerus evaluation of effective treatment (SPHEER) – what is the effect of rehabilitation compliance on clinical outcomes of proximal humerus fractures. BMC Musculoskeletal Disorders, 24, 778. https://doi.org/10.1186/s12891-023-06894-w
- Razaeian, S., Krettek, C., & Hawi, N. (2022). Algorithmus zur konservativen Behandlung von proximalen Humerusfrakturen: Erfahrungen aus dem Hannover Humerusregister. Obere Extremität, 17, 162–171. https://doi.org/10.1007/s11678-022-00702-y
- Razaeian, S., & Krettek, C. (2025). Nonoperative treatment of proximal humerus fractures in the elderly. European Journal of Trauma and Emergency Surgery, 51, 248-263. https://doi.org/10.1007/s00068-025-02912-9
- Spross, C., Meester, J., Mazzucchelli, R. A., Puskás, G. J., Zdravkovic, V., & Jost, B. (2019). Evidence-based algorithm to treat patients with proximal humerus fractures-a prospective study with early clinical and overall performance results. Journal of Shoulder and Elbow Surgery, 28(6), 1022-1032. https://doi.org/10.1016/j.jse.2019.02.015


