Rotator cuff (RC) repair is a commonly performed surgical procedure aimed at restoring shoulder function and reducing pain due to tendon tears. However, postoperative rehabilitation is equally crucial to the success of the surgery, ensuring appropriate healing and functional recovery. Given the variability in tear size, tissue quality, surgical technique, patient age, activity level, and comorbidities such as diabetes or smoking status, rehabilitation protocols must be tailored to each patient. A one-size-fits-all approach is inadequate because biological healing rates and risk factors differ significantly among individuals.
Communication between the surgical team and rehabilitation specialists is vital to customize the rehabilitation process based on:
- Tear size (small, medium, large, massive)
- Tendon quality and repair security
- Patient-specific factors (age, comorbidities, activity goals)
- Concomitant procedures (e.g., biceps tenodesis/tenotomy)
- Preoperative condition (e.g., stiffness, muscular atrophy)
This protocol integrates evidence-based recommendations and expert consensus to guide rehabilitation phases, precautions, and progression criteria, optimizing patient outcomes while minimizing complications such as re-tear or stiffness.
Rehabilitation Protocol Overview
The rehabilitation program is divided into five phases, each with defined goals, precautions, interventions, and progression criteria. Timelines may vary based on individual patient factors and tear severity.
Phase 0: Preoperative Preparation (If applicable)
- Goals: Optimize shoulder function pre-surgery; educate patient on postoperative expectations.
- Interventions: Preoperative physiotherapy focusing on scapular stabilization, rotator cuff strengthening, and maintaining range of motion.
- Precautions: Smoking cessation advised to improve tendon healing.
- Notes: Ensure patients understand the importance of compliance with postoperative protocols.
Phase 1: Immediate Postoperative Phase (Weeks 0–6)
Goals
- Protect the repair site and maintain integrity.
- Minimize pain and inflammation.
- Prevent stiffness by initiating safe range of motion.
- Educate patient on precautions and self-care.
Precautions
- Strict immobilization with sling or abduction brace (typically 4–6 weeks; longer for larger tears or poor tissue quality).
- Avoid active shoulder movements.
- No lifting or supporting weight with the operated arm.
- Avoid excessive stretching or forceful motions.
- For repairs involving the subscapularis tendon, limit external rotation to neutral to avoid excessive strain.
Modalities
- Cryotherapy: Frequent use (ice packs 15–20 minutes every 1–2 hours) to control pain and swelling.
- Electrical stimulation: May be considered to maintain muscle activation without stressing repair.
- Optional: Continuous passive motion (CPM) may be used, but offers no definitive long-term benefit over therapist-assisted passive motion.
Range of Motion (ROM)
- Initiate passive ROM (PROM) exercises within safe limits.
- Avoid PROM beyond:
- Forward elevation: 90° progressing to 120° by week 6.
- External rotation: 30° to 45° in scapular plane.
- Internal rotation: limited and avoiding aggressive stretching.
- Positions such as scapular plane abduction (~30° forward of frontal plane) are preferred to minimize tendon strain.
Exercises (examples)
- Pendulum exercises: Gentle small circles with trunk flexed forward to minimize muscular activation.
- Passive forward elevation: Therapist-assisted within pain-free range, performed in scapular plane.
- Passive external rotation: Therapist-assisted, limited to safe degrees.
- Scapular retraction and depression: Isometric activation with arm supported.
- Elbow, wrist, and hand active ROM: To prevent stiffness and promote circulation.
- Towel-assisted passive elevation: Patient uses towel to assist elevation in supine position.
- Aquatic therapy: Early gentle movements in water to aid pain-free ROM.
Notes
- Sling worn continuously except during exercises.
- Patients instructed on safe positioning, posture, and avoiding compensatory movements such as shoulder shrugging.
- Patients with biceps tenodesis or tenotomy: limit elbow flexion and supination movements initially to protect repair.
Criteria to progress to Phase 2
- Acceptable PROM: forward elevation ≥120°, external rotation ≥45°, internal rotation ≥45° (adjusted for contralateral side) [[118]].
- Pain controlled and minimal inflammation.
- Patient adherence with precautions.
Phase 2: Early Motion and Protection Phase (Weeks 6–12)
Goals
- Restore full passive and initiate active-assisted ROM.
- Begin reactivation of rotator cuff and scapular stabilizers with low-load exercises.
- Continue pain and inflammation management.
Precautions
- No heavy lifting (>5 lb) or sudden jerking movements.
- Avoid resistance exercises that produce high tendon strain.
- Monitor for signs of compensation or excessive muscle activation (e.g., shoulder shrug).
Modalities
- Continue cryotherapy as needed.
- Heat may be applied before exercises to improve tissue extensibility.
- Aquatic therapy with active movements encouraged.
Range of Motion (ROM)
- Progress active-assisted ROM (AAROM) and then active ROM (AROM) as tolerated.
- Focus on controlled movement in scapular plane.
- Avoid excessive external rotation in abduction if subscapularis involved.
Exercises (examples)
- Active-assisted forward elevation: Using pulley or wand, progressing to unsupported elevation.
- Active-assisted external rotation: Using wand or pulley at safe ranges.
- Scapular stabilization: Rhythmic stabilization drills at 90° elevation.
- Isometric rotator cuff exercises: Submaximal, pain-free contractions in neutral or scapular plane.
- Pendulum progressions: Larger circles or “forward bow” exercises.
- Therapist-assisted passive and active ROM: To aid in overcoming stiffness.
- Aquatic active ROM exercises: To allow movement with reduced gravity.
Notes
- Exercises should produce <30% maximal voluntary isometric contraction (MVIC) in supraspinatus to protect repair.
- Progression individualized based on pain, ROM, and strength.
- Patients with large or massive tears require more cautious progression, potentially delaying active motion and strengthening.
- Patients with biceps repairs require limited elbow motion initially.
Criteria to progress to Phase 3
- Full or near-full passive and active ROM without compensations.
- Pain minimal or absent during exercises.
- No signs of muscle inhibition or shoulder instability.
Phase 3: Intermediate Strengthening Phase (Weeks 12–20)
Goals
- Restore muscular strength, endurance, and neuromuscular control.
- Enhance scapulohumeral rhythm and dynamic stability.
- Initiate functional activities as tolerated.
Precautions
- Avoid high-load resisted exercises that cause pain or compensatory movements.
- Avoid sudden or ballistic movements.
- Monitor for signs of re-injury or overuse.
Modalities
- Continue cryotherapy or heat as needed.
- Initiate neuromuscular electrical stimulation if indicated.
Range of Motion (ROM)
- Maintain full active and passive ROM.
- Address residual stiffness with gentle stretching.
Exercises (examples)
- Isotonic strengthening with elastic bands: External and internal rotation at 0° abduction.
- Sidelying external rotation: Targets infraspinatus and teres minor.
- Prone rowing and horizontal abduction: Scapular and posterior cuff strengthening.
- Scapular stabilization drills: Closed kinetic chain exercises such as quadruped weight shifts.
- Forward flexion with light weights: Progress from gravity-assisted to resisted.
- Biceps and triceps strengthening: Light resistance curls and extensions.
- Rhythmic stabilization drills: At varying degrees of elevation to enhance dynamic joint stability.
Notes
- Progress resistance cautiously, avoiding supraspinatus activation >50% MVIC.
- Avoid exercises causing shoulder “shrug” sign (indicative of poor rotator cuff control).
- Consider patient-specific goals: laborers and athletes may require advanced strengthening.
- For massive tears, strengthening focuses on compensatory muscles and scapular stabilizers.
Criteria to progress to Phase 4
- Full pain-free ROM.
- Adequate strength and dynamic stability demonstrated.
- Patient able to perform fundamental functional tasks.
Phase 4: Advanced Strengthening and Functional Return (Weeks 20–26+)
Goals
- Maximize strength, endurance, and power.
- Restore full functional capacity for work and sport.
- Implement sport-specific or job-specific training.
Precautions
- Avoid overloading repair site; respect signs of pain or fatigue.
- Gradual return to high-demand activities.
- Avoid ballistic or plyometric exercises until adequate strength achieved.
Modalities
- Cryotherapy post-intensive sessions.
- Neuromuscular re-education as needed.
Exercises (examples)
- Advanced isotonic strengthening: External rotation at 90° abduction with resistance.
- Push-up plus: Enhances serratus anterior and scapular control.
- Wall slides and wall ball exercises: For scapulothoracic rhythm.
- Plyometric exercises: Light medicine ball throws, progressing to sport-specific throws.
- Interval sport programs: Golf, tennis, throwing progressions.
- Closed kinetic chain drills: Perturbations and weight shifts in standing or quadruped.
- Core strengthening: Integration of trunk and lower extremity to support shoulder function.
Notes
- Progression individualized; not all patients require this phase.
- Monitor for compensations or signs of overuse.
- Patients with biceps involvement may require delayed or modified strengthening.
Criteria for return to full activity
- Restoration of strength and endurance.
- Absence of pain or instability.
- Clearance from surgeon and therapist.
Additional Notes for Tear Size and Special Considerations
- Small-to-Medium Tears (<4 cm): Typically follow accelerated rehab with earlier motion and strengthening.
- Large Tears (4–5 cm): Rehabilitation is more conservative; sling use longer, delayed motion initiation, cautious strengthening.
- Massive Tears (>5 cm): May require extensive protection, focus on compensation, and possibly alternative treatments.
- Biceps Tenodesis/Tenotomy: Limit elbow flexion and supination initially; avoid active biceps strengthening until cleared.
- Subscapularis Repair: Limit external rotation and stretching in early phases to prevent excessive strain.
- Stiffness Management: If ROM lag or pain persists, emphasize gentle stretching, increased frequency of home exercises, and close communication with surgeon.
- Immobilization: Typically 4–6 weeks; longer immobilization may increase stiffness risk without improving healing.
- Continuous Passive Motion (CPM): Offers limited long-term benefit but may reduce early pain and assist in early ROM.
- Aquatic Therapy: Provides a low-load environment to facilitate active motion safely.
Summary Table of Phases and Timeline
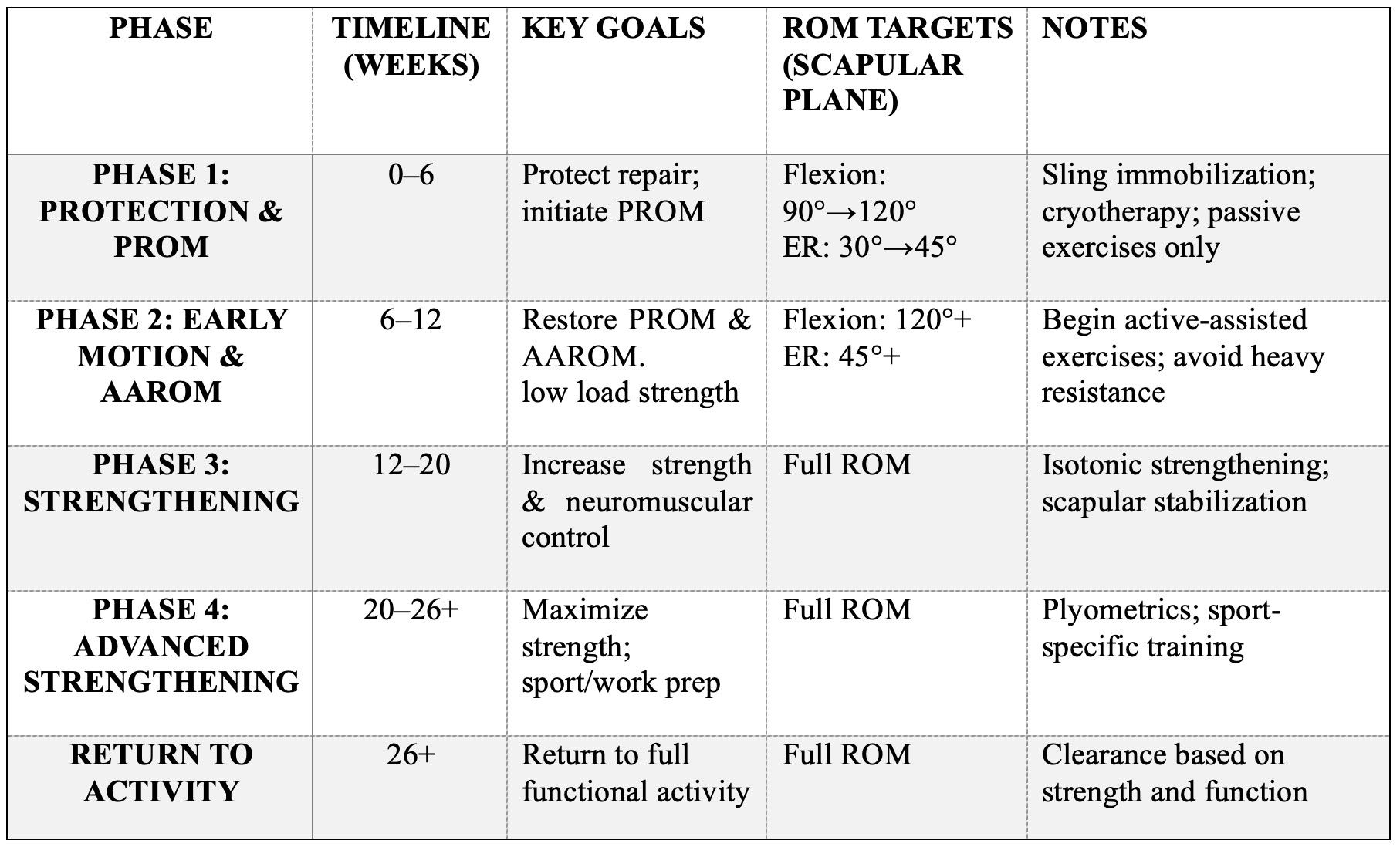
Key Points Summary
- Rehabilitation must be individualized considering tear size, tissue quality, surgery type, and patient factors.
- Immobilization for 4–6 weeks in abduction sling is standard, but prolonged immobilization may increase stiffness without improving repair integrity.
- Early passive ROM within safe ranges does not increase risk of re-tear and may reduce stiffness.
- Active motion and strengthening are cautiously introduced based on healing status and functional milestones.
- Electromyographic (EMG) studies guide exercise selection to minimize tendon strain during early rehab.
- Aquatic therapy is beneficial for early active ROM with reduced load.
- CPM provides limited benefit and is not superior to therapist-assisted passive motion.
- Patient education and adherence to restrictions are crucial to prevent complications.
- Biceps repairs and subscapularis involvement require specific modifications in rehab.
- Return to sport and high-demand activities may take 6–12 months and require sport-specific programs.
Reference:
- Sgroi, T. A., & Cilenti, M. (2018). Rotator cuff repair: post-operative rehabilitation concepts. Current Reviews in Musculoskeletal Medicine, 11(2), 86–91. https://doi.org/10.1007/s12178-018-9462-7
- Thomson, S., Jukes, C., & Lewis, J. (2016). Rehabilitation following surgical repair of the rotator cuff: a systematic review. Physiotherapy, 102, 20–28. https://doi.org/10.1016/j.physio.2015.08.003
- Wilk, K. E., Crockett, H. C., & Andrews, J. R. (2000). Rehabilitation after rotator cuff surgery. Techniques in Shoulder & Elbow Surgery, 1(2), 128–138. https://doi.org/10.1053/tses.2000.15012
- Millett, P. J., Wilcox, R. B., O’Holleran, J. D., & Warner, J. J. (2006). Rehabilitation of the rotator cuff: an evaluation-based approach. Journal of the American Academy of Orthopaedic Surgeons, 14(11), 599–609. https://doi.org/10.5435/00124635-200611000-00002
- Mazuquin, B., Moffatt, M., Gill, P., et al. (2021). Effectiveness of early versus delayed rehabilitation following rotator cuff repair: Systematic review and meta-analyses. PLoS ONE, 16(5), e0252138. https://doi.org/10.1371/journal.pone.0252138
- Thigpen, C. A., Shaffer, M. A., Gaunt, B. W., et al. (2016). The American Society of Shoulder Therapists’ consensus statement on rehabilitation following arthroscopic rotator cuff repair. Journal of Shoulder and Elbow Surgery, 25(3), 521–535. https://doi.org/10.1016/j.jse.2015.12.018
Please note: This rehabilitation protocol should be adapted to the individual patient’s clinical presentation and in consultation with the surgical team. The exercises listed are examples; therapists should select and modify based on patient tolerance and progression.