Hip arthroscopy has become an increasingly popular, minimally invasive surgical technique to address intra-articular hip pathologies such as femoroacetabular impingement (FAI), labral tears, and chondral injuries, particularly in young and athletic populations. The goal is to reduce pain and restore function, enabling athletes to return to sport safely and effectively.
Femoroacetabular impingement syndrome (FAIS) is a condition characterized by abnormal and dynamic contact between the femoral head–neck junction and the acetabular rim, caused by altered bone morphology such as cam, pincer, or mixed types. This abnormal contact results in progressive damage to the acetabular labrum, chondrolabral junction, and articular cartilage, potentially leading to hip joint degeneration and osteoarthritis. Diagnosis of FAIS is based on a triad of patient symptoms (such as pain, clicking, stiffness, and limited range of motion), specific clinical maneuvers (including the flexion adduction internal rotation and flexion abduction external rotation tests), and imaging studies (orthogonal hip and pelvis X-rays, and MRI or arthrograms). Initial treatment is often conservative, involving physical therapy, intra-articular injections, and activity modification. When conservative management fails or specific criteria are met, surgical treatment, primarily hip arthroscopy, which is a minimally invasive surgical procedure, is performed to correct bony abnormalities and repair or reconstruct labral lesions, aiming to preserve hip function and alleviate symptoms.
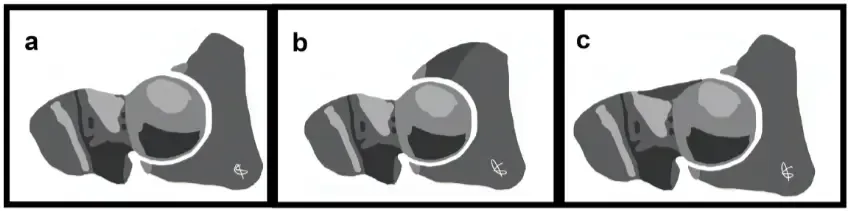
Schematic representation of hip: (a) normal hip, (b) hip with pincer-type impingement (the dark gray zone represents the acetabular over-coverage), and (c) hip with cam-type impingement (the dark gray zone represents the femoral head-neck junction abutment).
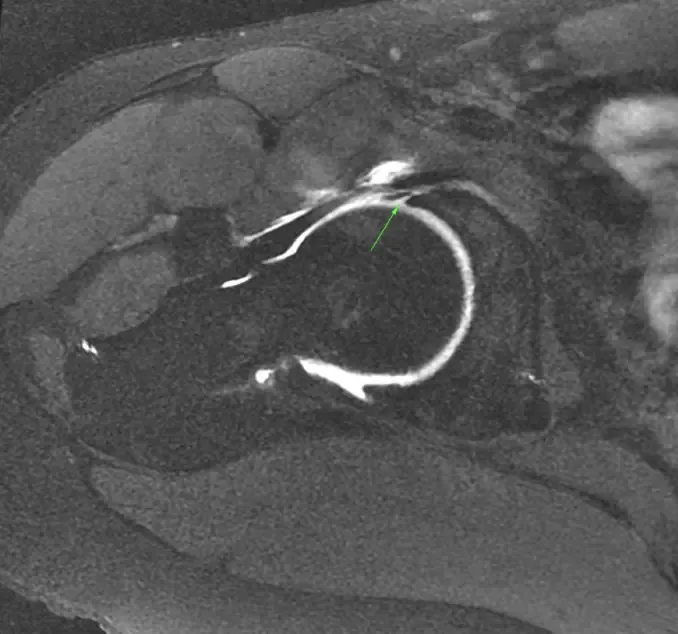
Effective postoperative rehabilitation is crucial to optimize surgical outcomes, restore function, and facilitate a safe return to sport or daily activities. The following protocol synthesizes current evidence and expert consensus on rehabilitation following hip arthroscopy, organized into distinct phases with detailed goals, interventions, precautions, and progression criteria. This comprehensive framework integrates findings from multiple systematic reviews, clinical studies, and expert guidelines.
Phase 1: Immediate Post-Operative Phase (0–2 Weeks)
Goals:
- Protect surgical repair and promote healing
- Control pain and inflammation
- Prevent muscle inhibition and atrophy
- Maintain gentle range of motion (ROM) within safe limits
- Educate patient on precautions and safe mobility
Interventions:
- Use of hip brace limiting flexion >90° and abduction beyond neutral when indicated (e.g., labral repair, capsular closure)
- Pain control modalities (cryotherapy)
- Patient education on weight-bearing restrictions, use of assistive devices (crutches), and activity modification
- Isometric activation of gluteal muscles, quadriceps, transverse abdominis (with diaphragmatic breathing), and deep hip rotators
- Passive ROM exercises such as circumduction and gentle hip rotations within limits
- Avoid active hip flexion and excessive extension to protect anterior capsule and labrum
Weight-Bearing:
- Flat-foot partial weight bearing (PWB) of approximately 20 lbs for 2 weeks; extended to 4–6 weeks if microfracture or cartilage repair performed
- Progression to weight-bearing as tolerated (WBAT) after 2 weeks if no microfracture
Precautions:
- Avoid hip flexion beyond 90°, extension beyond neutral, excessive abduction, and rotation beyond 20° for 3–4 weeks
- Prevent hip flexor tendonitis by limiting activation of secondary hip flexors
- Avoid prolonged sitting, especially with hip flexion and crossed legs
Criteria to Progress:
- Pain controlled and minimal
- Compliance with weight-bearing and brace use
- Ability to perform prescribed isometric exercises without pain
- Safe ambulation with assistive devices
Phase 2: Early Rehabilitation Phase (2–6 Weeks)
Goals:
- Restore pain-free full or functional ROM
- Normalize gait pattern without assistive devices
- Begin gentle strengthening focusing on neuromuscular control
- Prevent muscle atrophy and adhesions
Interventions:
- Progress from isometric to isotonic strengthening exercises excluding hip flexors initially.
- Initiate weight-shifting, heel/toe raises, and double-leg stance exercises.
- Introduce aquatic therapy (e.g., chest-deep walking) to facilitate low-impact cardiovascular training and improve ROM.
- Continue soft tissue mobilization and manual therapy to maintain hip mobility.
- Stationary bike with low resistance, adjusted saddle height to avoid excessive hip flexion.
- Gentle stretching of hip capsule and periarticular muscles (quadriceps, piriformis, adductors) within pain tolerance.
Weight-Bearing:
- Progress to WBAT, typically by 4 weeks post-op.
Precautions:
- Avoid deep hip flexion movements (e.g., low lunges), excessive stretching, and rotational activities causing pain.
- Avoid treadmill or high-impact activities.
Criteria to Progress:
- Full, pain-free ROM or functional ROM sufficient for daily activities
- Normal gait without limp
- Hip flexor strength at least 4−/5 and other hip muscle strength at least 4/5 by manual testing.
- Ability to perform weight-bearing exercises without pain or compensation
Phase 3: Strengthening and Neuromuscular Control Phase (6–12 Weeks)
Goals:
- Restore hip muscle strength, especially abductors, extensors, and rotators
- Improve dynamic balance and neuromuscular control
- Enhance cardiovascular endurance
- Begin gradual return to functional activities
Interventions:
- Begin more advanced strengthening exercises, such as squats and deadlifts (start with double-leg and progress to single-leg around weeks 8–10), as well as lunges and step-ups.
- Incorporate core strengthening exercises: planks, bridges.
- Begin proprioceptive and balance exercises on stable and unstable surfaces.
- Cardiovascular training with elliptical, swimming (without kicking initially), and walking.
- Plyometric exercises initiated cautiously, focusing on technique and control.
Weight-Bearing:
- Full weight-bearing without assistive devices.
Precautions:
- Avoid contact sports, high-impact, and rotational activities that cause pain or instability.
- No aggressive hip flexor strengthening until adequate healing and strength achieved.
Criteria to Progress:
- Strength ≥ 80% of contralateral side in key hip muscle groups.
- Good dynamic control demonstrated in single-leg tasks
- Cardiovascular endurance adequate for increased activity
- No pain or compensatory movement during strengthening and functional exercises
Phase 4: Advanced Functional and Return to Sport Phase (12+ Weeks)
Goals:
- Achieve pre-injury or better hip strength and endurance
- Enhance power, agility, and sport-specific skills
- Ensure psychological readiness for return to activity
Interventions:
- Advanced plyometrics, agility drills (ladder drills, carioca, zig-zag running).
- Sport-specific drills tailored to individual’s demands.
- Continued core and hip strengthening with increased resistance and complexity.
- Functional testing (Y-balance test, hop tests, single leg squat quality) to assess readiness.
- Address psychological factors such as kinesiophobia using validated scales (e.g., Tampa Scale of Kinesiophobia)
Weight-Bearing:
- Unrestricted weight-bearing and activity as tolerated.
Precautions:
- Avoid returning to sport prematurely to prevent recurrence of symptoms.
- Monitor for pain, swelling, or functional deficits during progression
Criteria to Progress/Return to Sport:
- Passing functional criteria: >85% on Hip Outcome Score – Sport Subscale, >80% limb symmetry on strength and balance tests.
- Pain-free performance of sport-specific tasks
- Psychological readiness confirmed
Note: If your goal is to return to sport or a higher level of physical activity, please read our Return to Sport Article.
Summary Table of Rehabilitation Phases After Hip Arthroscopy
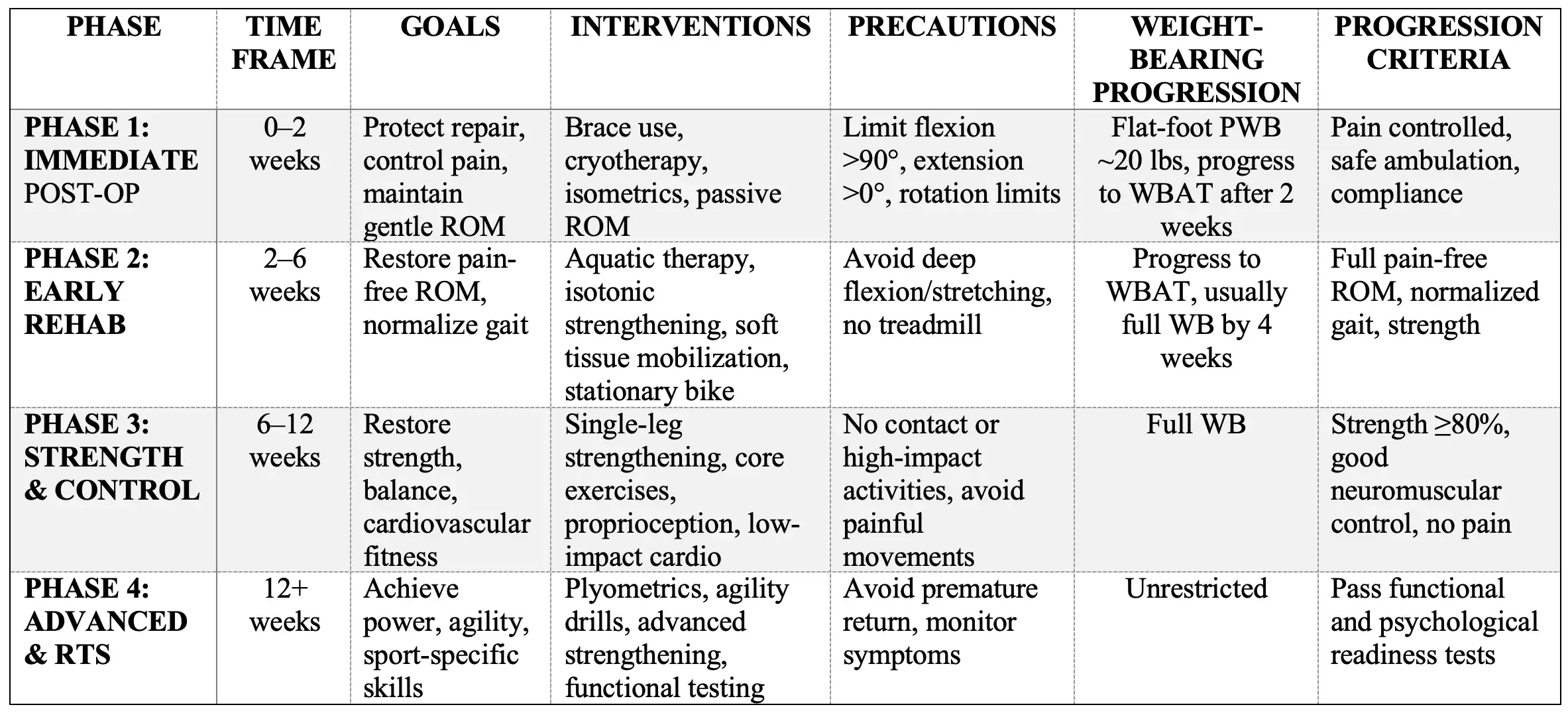
Reference:
- Reference: Gómez-Verdejo, F., Alvarado-Solorio, E., & Suarez-Ahedo, C. (2025). Review of femoroacetabular impingement syndrome. Journal of Hip Preservation Surgery, 11(4), 315–322. https://doi.org/10.1093/jhps/hnae034
- Ankem, H. K., Yelton, M. J., Lall, A. C., Bendersky, A. M., Rosinsky, P. J., Maldonado, D. R., Meghpara, M. B., & Domb, B. G. (2020). Structured physical therapy protocols following hip arthroscopy and their effect on patient-reported outcomes—a systematic review of the literature. Journal of Hip Preservation Surgery, 7(3), 357–377. https://doi.org/10.1093/jhps/hnaa042
- Bistolfi, A., Guidotti, C., Aprato, A., Sabatini, L., Artiaco, S., Massè, A., & Ferracini, R. (2021). Rehabilitation protocol after hip arthroscopy: A 2015–2020 systematic review. American Journal of Physical Medicine & Rehabilitation, 100(10), 958–965. https://doi.org/10.1097/PHM.0000000000001677
- Disantis, A., Bonin, N., Byrd, T., Campbell, A., Christoforetti, J., Dienst, M., Ellis, T., Enseki, K., Kivlan, B., Kohlrieser, D., Lifshitz, L., Manske, R., McClincy, M., O’Donnell, J., Safran, M., Takla, A., Tyler, T., Voight, M., & Martin, R. (2025). The 2024 International Society for Hip Preservation physiotherapy agreement on post-operative rehabilitation following hip arthroscopy for femoroacetabular impingement syndrome. Journal of Hip Preservation Surgery, 00(00), 1–7. https://doi.org/10.1093/jhps/hnaf055
- Domb, B. G., Sgroi, T. A., & VanDevender, J. C. (2016). Physical therapy protocol after hip arthroscopy: Clinical guidelines supported by 2-year outcomes. Sports Health, 8(4), 347–354. https://doi.org/10.1177/1941738116647920
- Grzybowski, J. S., Malloy, P., Stegemann, C., Bush-Joseph, C., Harris, J. D., & Nho, S. J. (2015). Rehabilitation following hip arthroscopy – a systematic review. Frontiers in Surgery, 2, 21. https://doi.org/10.3389/fsurg.2015.00021
- Hemstock, R., Mulhall, D., Didyk, J., Ogborn, D., & Lemmex, D. (2023). Postoperative weight-bearing restrictions and rehabilitation protocols after hip arthroscopy for femoroacetabular impingement: A systematic review. Journal of Hip Preservation Surgery, 10(3-4), 220–227. https://doi.org/10.1093/jhps/hnad023
- Monselli, C., Bianco Prevot, L., Accetta, R., Tronconi, L. P., Bolcato, V., & Basile, G. (2024). State of the art in rehabilitation strategies after hip arthroscopy for femoroacetabular impingement syndrome: A systematic review. Journal of Clinical Medicine, 13(7302), 1–13. https://doi.org/10.3390/jcm13237302
- Reiman, M. P., Boyd, J., Ingel, N., Sylvain, J., Peters, S., & Ayeni, O. R. (2020). There is limited and inconsistent reporting of postoperative rehabilitation for femoroacetabular impingement syndrome: A scoping review of 169 studies. Journal of Orthopaedic & Sports Physical Therapy, 50(5), 252–258. https://doi.org/10.2519/jospt.2020.9189
- Diemer, F., Zebisch, J., Zinser, W., Steens, W., Zimmerer, A., & Schoch, W. (2025). Physiotherapy and exercise therapy after surgical treatment of femoroacetabular impingement syndrome: A clinical commentary from the QKG – Society for Cartilage Regeneration and Joint Preservation. International Journal of Sports Physical Therapy, 20(11), 1653–1669. https://doi.org/10.26603/001c.146239

